1.
ottawa paramedic
service –– 2006 ANNUAL REPORT AND 2007 PERFORMANCE TRENDS SERVICE PARAMÉDIC D’OTTAWA – RAPPORT
ANNUEL DE 2006 ET TENDANCES DU RENDEMENT DE 2007 |
COMMITTEE
RECOMMENDATION
That Council receive this report for information.
Recommandation
du comité
Que leConseil reçoivent ce rapport aux fins d’information.
For
the information of Council
The Committee approved the following direction to staff:
That Tony Di Monte, Chief of the Ottawa Paramedic Service and Community
and Protective Services Committee Chairperson Deans to meet with
Dr. Kitts, President and Chief Executive Officer of the Ottawa Hospital,
Dr. Cushman, Chief Executive Officer of the Champlain Local Health Integration
Network (LHIN) and the Provincial and Federal Ministers of Health, to discuss
strategies to free up hospital beds to reduce hospital wait time for paramedics
and report back to the Community and Protective Services Committee.
And that Chief Di Monte and Chair Deans be directed to go to a LHIN
Board meeting to encourage them to exercise their power in this regard.
Pour
la gouverne du Conseil
Le Comité a approuvé la directive suivante à l’intention du
personnel :
Que Tony Di Monte, chef du Service paramédic d’Ottawa, et que madame Deans,
présidente du Comité des services communautaires et de protection, rencontrent
le Dr Kitts, président-directeur général de l’Hôpital d’Ottawa, le Dr
Cushman, directeur général du Réseau local d’intégration des services de santé
de Champlain (RLISS) ainsi que les ministres provincial et fédéral de la Santé,
afin de discuter de stratégies permettant de libérer des lits d’hôpital et
réduire le temps d’attente du service paramédic, et de rendre compte au Comité
des services communautaires et de protection.
Et que le chef Di Monte et la présidente
Deans soient chargés d’assister à une réunion du conseil d’administration du
RLISS afin d’inciter ses membres à exercer leur pouvoir à cet égard.
DOCUMENTATION
1.
Deputy
City Manager, Community and Protective Services report dated 5 October 2007 (ACS2007-CPS-OPS-0002).
2.
Extract
of Minute, 18 October 2007.
Report to/Rapport au :
Community Protective Services Committee
Comité des services communautaires et de protection
and Council / et au Conseil
5 October 2007/le 5 octobre
2007
Submitted by/Soumis par : Steve Kanellakos,
Deputy City Manager/Directeur municipal adjoint,
Community and Protective Services/Services communautaires et de
protection
Contact Person/Personne ressource : Anthony Di
Monte, Chief / Directeur
Ottawa
Paramedic Service/Services paramédic d’Ottawa
(613)
580-2424 x22458, Anthony Di Monte@Ottawa.ca
|
SUBJECT: |
ottawa paramedic service ––2006 ANNUAL REPORT AND
2007 PERFORMANCE TRENDS |
|
OBJET: |
SERVICE PARAMÉDIC D’OTTAWA – RAPPORT ANNUEL DE
2006 ET TENDANCES DU RENDEMENT DE 2007 |
REPORT
RECOMMENDATION
That Community and Protective Services Committee and Council receive this report for information.
RECOMMANDATION DU RAPPORT
Que les Services communautaires et de
protection ainsi que le Conseil reçoivent ce rapport aux fins d’information.
In
response to the recommendations emanating from the Coroner’s
Inquest into the death of Alice V. Martin as well as the 2004 mid year report
(ACS2004-CPS-OPS-0008),
Council approved the addition of 52 paramedic
FTEs over 2 years. The last 18
staff were hired in July of 2006. As part
of the same report, the recommendation was approved “that staff report back to
Committee and Council prior to budget each year on performance trends,
mitigation strategies and associated
financial impacts to ensure the service can maintain its baseline performance
targets”.
The following report provides statistics
for 2006 for call volume;
response time and hospital wait time as directed by Council. It also identifies trends for 2007 and
illustrates potential staffing strategies to address the growing problem over
the next three year.
RÉSUMÉ
In October 2004, the Ottawa Paramedic Service
reported to the former Emergency and Protective Services Committee and Council
on call volume, hospital wait time and response time trends. That report indicated that in 2003 and 2004,
rising call volumes surpassed the capacity of the service, resulting in
increased response times in both the urban and rural sectors.
In response to the Coroner’s Inquest into the death
of Alice V. Martin recommendations as well as the 2004 mid year report, Council
approved the addition of 52 paramedic FTEs over 2 years. The last 18 staff were hired in July of
2006.
Based on data available for 2006, call volume reached 92,55488,732, which is significantly higher
than the assumption of the original system design of 65,000 requests for
service per year with annual anticipated increases of 2% per year. While
tWhilehe
overall call volume between 2005 and 2006 went downup
only marginally more than the projected 2%, the the
total number of calls remains significantly higher than the projected 73,200
for 2006. number
of code 4 calls (life threatening calls) rose dramatically by almost
22%.
Table
1: Call Volume
|
Call Volumes |
|||||||
Call Type
|
2001 |
2002 |
2003 |
2004 |
2005 |
2006 |
2007 Projected |
|
Code 4 |
36,753 |
42,915 |
49,283 |
55,890 |
|||
|
Code 3 |
20,662 |
22,601 |
21,569 |
20,974 |
22,200 |
12,409 |
12,879 |
|
Code 2 |
4,578 |
4,873 |
4,616 |
6,576 |
6,324 |
5,597 |
7,073 |
|
Code 1 |
10,457 |
9,467 |
7,335 |
6,618 |
4,350 |
3,011 |
2,592 |
|
Code 8 |
N/A |
N/A |
N/A |
N/A |
N/A |
1,758[1] |
2,272 |
|
Total |
72,450 |
79,856 |
82,803 |
90,058 |
90,140 |
92,554 |
97,339 |
|
Source :
MOHLTC |
|||||||
This increase in code four (4)
can be attributed in part to the new Computer Aided
Dispatch system implemented in 2006 and
its new categorization of calls;
however, it can also be attributed to population growth and its aging at a
disproportionate rate with the elderly making use of the
service far more often than younger people.
In 2006,
stroke, heart problems, shortness of breath and falls – ailments normally
associated with the elderly - accounted for approximately 30% of all calls. This
represents an increase of approximately 3700
calls associated with the elderly in 2006. These
code 4 calls require a more sophisticated and time consuming intervention by
paramedics placing further demand on the paramedic system. Unlike
lower priority calls (code 1 & 2), which can be planned and scheduled, the
severity of these calls requires an
immediate response depleting resources.
According to the Corporate Environmental Scan
completed in 2006, the senior population (65+) in Ottawa will likely increase
by at least 50% over the next 20 years, and will represent slightly over 16 %
of total population in 15 years. The very elderly, 85+, will increase by 25% in
the next five years, accelerating demands on paramedic services, health care,
and long term care facilities.
The shortage of family physicians, long wait times for emergency rooms and the enhanced medical care provided by paramedics are all contributing to a public perception and reliance on the Paramedic Service as a provider of primary health care.
In
2006, the number of code 4 – life-threatening calls have increased sharply. The code 4 calls require a more sophisticated
and time consuming intervention by paramedics placing further demand on the
paramedic system. Unlike lower priority
calls (code 1 & 2), which can be planned and scheduled, the severity of
these calls requires the immediate response depleting resources. The shortage
of family physicians, long wait times for emergency rooms and the enhanced
medical care provided by paramedics are all contributing to a public perception
and reliance on the Paramedic Service as a provider of primary health
care. Despite these trends it appears
that Ottawa is experiencing a levelling out of calls for service in 2005 and
had a slight decrease in demand for service in 2006.
Although it was never achieved in Ottawa, when the paramedic deployment model was originally developed, the provincial standard for the return to service of a paramedic crew after arrival at hospital (hospital wait time) was twenty (20) minutes on average. Recently, a recommendation has been put forward from Dr. Brian Schwartz of The Hospital Emergency Department and Ambulance Effectiveness Working Group to change the provincial standard for hospital wait time to thirty minutes (30) at the 90th percentile - a more stringent standard. Across Canada, Paramedic Services are experiencing an increase in hospital wait time. In Ottawa in 2006, the average wait time was 53 minutes and 31 seconds – an increase of 3 minutes and 36 seconds from the previous year. An increasing wait time negatively impacts response time and paramedic availability given that paramedic crews are not available for assignment or deployment until the patient has been transferred into the care of hospital staff.
The following tables illustrate increases in hospital wait times since 2001 both at the average and the 90th percentile and indicate another potentially significant increase in 2007 based on data available for the first six months.
Table 2: Average Hospital Wait time
|
|
2001 |
2002 |
2003 |
||||
|
Wait Time |
00:36:44 |
00:39:17 |
00:42:27 |
00:49:00 |
00:49:55 |
00:53:31 |
00:57:38 |
|
Source: MOHLTC |
|||||||
Table 3: Hospital Wait time 90th Percentile
|
|
2001 |
2002 |
2003 |
||||
|
Wait Time |
1:04:49 |
1:07:02 |
1:10:07 |
1:12:14 |
1:15:52 |
1:15:48 |
1:20:24 |
|
Source: MOHLTC |
|||||||
Based on the tables above, Ottawa well exceeds the provincial standard for hospital wait times of 30 minutes at the 90th percentile. In fact, in 2006 the hospital wait time was approximately 45 minutes above the standard, which accounts for approximately 4 ambulances which are routinely at the hospital and unavailable to receive the next call.
A number of initiatives have been undertaken to mitigate the lengthening hospital wait time in Ottawa. Participation on regional committees such as the Eastern Ontario Emergency Services Committee has resulted in the implementation of internal hospital procedures intended to expedite the transfer of patient care. As well, to provide for the equitable distribution of patients to health care facilities, the Ottawa Central Ambulance Communication Centre now directs Paramedic crews to particular hospitals in a structured manner designed to avoid the overload of any one emergency department (Patient Priority System). This system takes into account the hospital capacity and the acuity and type of care the patient requires.
Although solutions to the current hospital wait time is the
sole responsibility of the hospital administration, it remains a contributory
factor in paramedic availability and therefore negatively impacts service
response time.
Response time targets were developed for the City of Ottawa taking into account international industry standards, medical appropriateness, and community expectations. The performance targets are set at 8 minutes 59 seconds 90% of the time for life threatening calls in Ottawa’s high-density area and set at 15 minutes 59 seconds 90% of the time for life threatening calls in Ottawa’s low-density area[2].
These targets were reconfirmed by Council and reiterated by the recommendations of the Coroner’s jury into the death of Alice V. Martin.
In order to meet response time targets, there must
be enough Paramedics available, assigned, and deployed according to strict
parameters related to call demand (call volume), and call location (geography)
– known as system capacity.
|
Annual Call Volume |
||||||
|
65,000 |
||||||
|
72,450 |
||||||
|
79,856 |
||||||
|
82,803 |
||||||
|
90,058 |
||||||
|
90,140 |
||||||
|
92,554 |
||||||
With
call volume levelling out and potentially declining, hospital wait time being
addressed with a promising Provincial solution and response time on the
downward trend, only one other component of system capacity needs to be addressed
– paramedic availability.
|
Year |
Number
of Paramedics assign to the Urban area |
Number
of Code 4 calls In
the Urban area |
Number
of code 4 calls per paramedic In
the Urban area |
Response
time in the urban area |
|
2001 |
166 |
34,551 |
208 |
12:24 |
|
2002 |
180 |
40,340 |
224 |
10:50 |
|
2003 |
180 |
46,426 |
257 |
11:05 |
|
2004 |
188 |
52,537 |
279 |
12:06 |
|
2005 |
208 |
53,830 |
258 |
12:00 |
|
2006 |
224 |
65,592 |
293 |
12:32 |
Despite
the best efforts and optimal deployment, without continued investment to
increase staffing, the rising call volume and specifically the anticipated
rising number of code 4 calls will continue to surpass capacity and continue to
result in rising response times.
Paramedic
Availability
“Levels”
is a term used to describe availability of paramedic units. For example, Level 15 denote that there are
15 ambulances available to respond to calls for service. Level 4 refers to the fact that there are
only 4 ambulances available to respond.
As ambulances are deployed to calls, the number of remaining available
ambulances goes down and the level drops.
As the level goes down, staff invoke protocols to ensure all staff are
alerted and where appropriate attempt to take remedial action. The following table provides a high level
overview of the protocols for dealing with a declining “level” of service.
Table
3: Tony we need more detail in the protocol section
|
|
|
The
instances of “Level 0” are not recorded
in the
CAD system but are indicated by manual intervention through the Service’s
paging system. Since the pager is not
an analytical tool but rather a alerting system, analysis of the historical
level 0 will be time consuming and manual based on the limited amount of stored
data and capability of the tool. Staff
will need to review records of calls in the CAD system manually for times of
day that match the instance of “Level 0” still stored in the pager system. They will
then
need
to analyze what was going on at the time to cause the reduction in service
level. Ottawa
Paramedic Service has assigned staff to this task and over the next several
weeks will be working on this task
exclusively. They will then be able to provide a detailed
analysis
of
the instances of reduced services and recommendations to mitigate
The
number of ambulances available to respond to the next call is ever changing
given the random pattern of 911-call reception. Because of this unpredictable
nature of emergency calls, extreme weather events, or a combination of these
factors, the fleet may be engaged in its entirety, leaving no Paramedics to
respond - referred to as “Level Zero”.
It
is understood that extraordinary situations like sudden ice storms such as the
one experienced in Ottawa on December 22, 2006, can outweigh a system’s
capacity for a short period of time, however this should be on an exceptional
basis and should not be the norm.
Likewise, one may not want to staff the system permanently for these
situations as it would be cost prohibitive, but the system should be able to
respond to the normal demands of the community.
Inter-municipal
Comparisons
It
is difficult to compare Ottawa Paramedic Service with other Paramedic Services
in the country, as each service is unique in their collective agreements,
scheduling practices and deployment models. Ottawa has a particular challenge due
to its large geographic size requiring considerable more
resources compared to other urban cities to achieve the same response time
targets. In fact Toronto, Calgary and Edmonton combined could
fit within Ottawa’s geographic boundaries.
Below is a
table that shows comparisons between Ottawa and other municipalities. Ratios of paramedics to calls, population
and sq kilometres have been used to allow for comparison purposes.
Table 7:
Inter municipal Comparators
City
|
Geographic
Area |
Population
|
Number
of Paramedics
|
Total
number of Calls
|
Number of calls per paramedic
|
Number of citizens per paramedic
|
Number of sq kilometres per
paramedic
|
Year
|
BC (Lower Mainland)
|
2,878
|
2,116,581
|
1,079
|
208,126
|
193
|
1961
|
2.7
|
2007
|
Toronto
|
642
|
2,600,000
|
892
|
293,215
|
329
|
2914
|
.7
|
2006
|
Montreal
|
744
|
2,240,000
|
884
|
266,362
|
301
|
2533
|
.8
|
2006
|
Calgary
|
726
|
974,000
|
348
|
96,442
|
277
|
2798
|
2.1
|
2006
|
Edmonton
|
700
|
740,578
|
319
|
63,791
|
200
|
2321
|
2.2
|
2006
|
Ottawa
|
2,700
|
877,280
|
312
|
92,554
|
297
|
2811
|
8.7
|
2006
|
Ottawa (Urban)
|
426
|
831,000
|
224
|
87,527
|
391
|
3709
|
1.9
|
2006
|
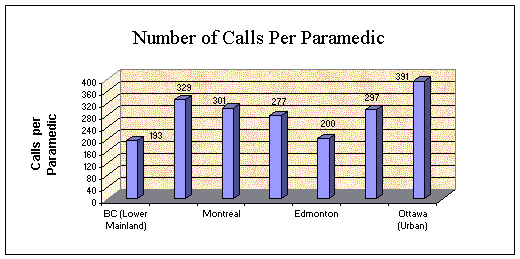
Both Edmonton and Calgary currently experience response
times in the 8 – 9 minute range.
However, as shown in the table above, each Ottawa paramedic responds to
significantly more calls than Edmonton and Calgary in addition to being
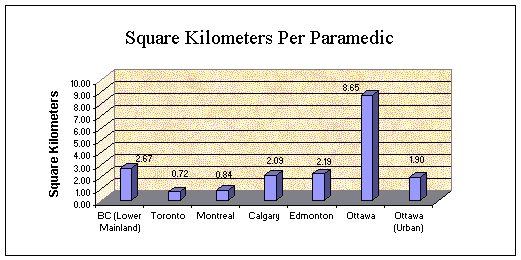
deployed over a significantly larger number of square kilometres. In
all instances, other cities have one paramedic per one to two kilometres. Ottawa has one paramedic per approximately 9
km kilometres. There comes a point in time
where sheer distance to travel is such that without sufficient resources, it is
physically impossible to respond within the targeted time frame. The following charts graphically
illustrates the comparison of Ottawa Paramedic Services with others in Canada.
Inter-municipal
Comparisons
It
is difficult to compare Ottawa Paramedic Service with other Paramedic Service
in the country, as each service is unique in their collective agreements,
scheduling practices and deployment models. Some services follow static and
more
costly deployment models as well.
Likewise, Ottawa geographical makeup always makes deployment of a
service more difficult given the vast area requiring coverage. However, conversations with other services
indicated that that “Level 0” is experienced only during abnormal situations
such as disasters or severe weather conditions and not part of regular
operations due to their staffing ratio.
Staffing
Ratio
The
nature, frequency and timing of emergency calls are unpredictable by
definition. Rarely are calls
received in alignment with exactly when an ambulance returns to service after
completing an assignment.
Consequently, if Ottawa Paramedic Service deploys 10 paramedic units
during the day and 10 calls are received in the first hour of the shift, there is
no available ambulance to attend the 11th
call. Despite staffing appropriately to
deal with busier times of the day, this situation does happen. In an effort to build in redundant resources
to ensure sufficient availability except in extreme circumstances,
the Paramedic industry developed a standard staffing ratio. In a static deployment model, staffing
should be such that 2/3rd
of the on shift resources are in excess of what call trends would demand –
therefore being available to deal with any inundation
of calls. For example, if 10 calls per
hour are normally received and each call takes an hour, there should be 30
ambulances on shift - Ten (or 1/3) ambulances to answer the first 10 calls, and
twenty ambulances (or 2/3) to be available for subsequent calls.
The
following chart indicates the number of calls received by Paramedic Service on
an average day and the number of resources required to deal with the calls
assuming a 2/3 redundancy.
Table
4:
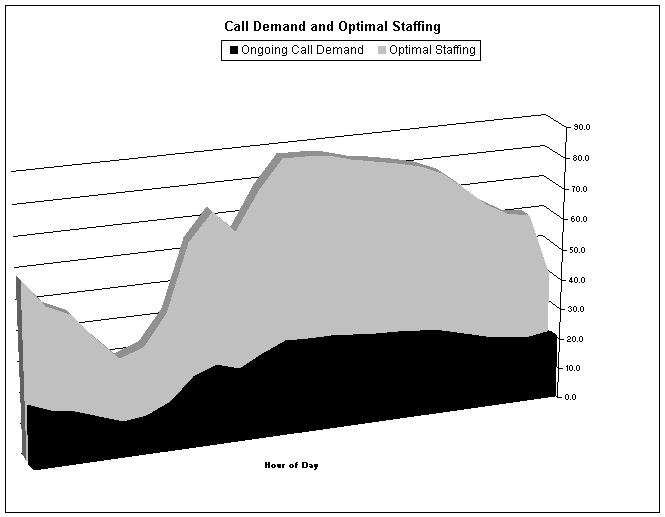
As
depicted in
table 4, significant resources would be required over an above the normal call
volume to ensure a 2/3 redundancy factor and mitigate the occurrence of reduced
levels of service – “level 0”
Table
5 shows the calls received on an average day for Paramedic
Service (bottom curve), the response capacity required to ensure 2/3 redundancy
factor (top curve) and the current level of staffing available within existing
Ottawa Paramedic Service resources (middle curve).
Table
5:
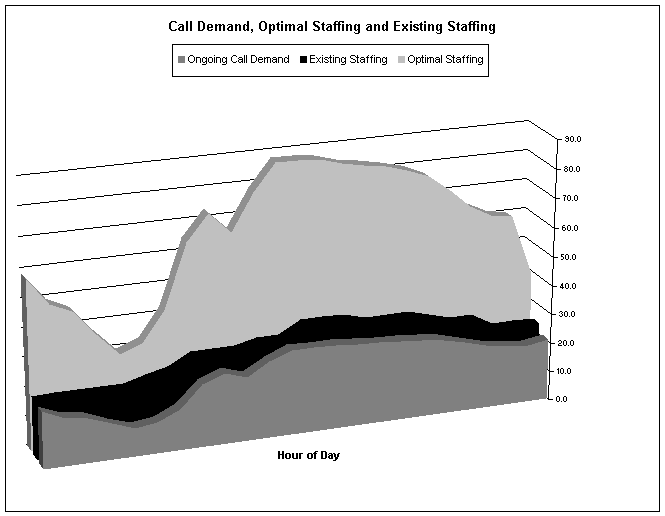
Although
the curve of resources deployed (middle curve) is closely aligned with (calls
for service) (bottom curve), which indicates that existing resources are
deployed appropriately to address the somewhat
predictable
trends of calls, the response capacity to
ensure a 2/3 redundancy factor is well above what currently exists in
Ottawa. There are simply not enough
available resources in Ottawa to deploy to this level of insurance. Currently there is little on shift surplus
to respond to any random influx of calls. As a result Ottawa does find itself at level
0
not only as a result of extreme circumstances but unacceptably as part of a
regular business day.
If
Ottawa were to consider staffing to a 2/3rd
redundancy factor, significant additional resources would be required. Currently,
each emergency call takes approximately 1 hour exclusive of hospital wait
time. Assuming that hospital wait time
is reduced to 30 minutes as a result of the new hospital pilot project which is
higher than the original system design
but lower than it has ever been in Ottawa since amalgamation, the time required
to complete an emergency (code 3 or code 4) call in the future will be
approximately 1 ½ hour.
Ottawa
Paramedic Service receives approximately 10 calls per hour on average per
day. Since calls take approximately 1.5 hours to complete, paramedics need
enough staff to respond to 15 calls per hour ((10 X 90 min)/60 min = 15 calls
per hour). Therefore, to achieve a 2/3rd
redundancy factor per industry standard, Ottawa would need to have 45 paramedic units
deployed on average per day - 15 units to deal with current calls (1/3rd)
and 30 as a redundancy to deal with a potential influx of calls (2/3rd). 15 of the remaining 30 will deal with the
next 1.5 hours of calls with remaining
15 resources available to respond to an influx of calls. It is important to note that those 15
“redundant” resources would be expected to cover the entire City (2700 sq km)
while the others are occupied on calls.
Currently,
Ottawa has 27 paramedic
units deployed on average per day (although distributed differently to address
periods of the day that see more calls than others see Table 5). Consequently, Ottawa would require an
additional 18 to meet these criteria with a static deployment model. This
is not what is required in Ottawa.
Since Ottawa utilizes
a more efficient dynamic deployment model where resources are deployed based on
location and trend of calls, a much lower redundancy factor is required.
However, to determine the true requirement
will take a period of time for staff to analyze the instances of level 0 and
the causes for it
as well as what type of redundancy factor would address
the need in Ottawa.
The City under a contract with the Province of
Ontario runs the Central Ambulance Communication Centre (CACC). In January of 2006, the Province replaced
the Computer Aided Dispatch system in Ottawa’s Communication Centre with a new
application resulting in a new code 8 type of call - which are emergency
standby calls received from Police and Fire where paramedics are required to
attend a call and standby in case of required medical care.
Provincial Cost Sharing
The Ottawa Paramedic Service receives a funding grant
from the Province of Ontario to operate the Central Ambulance Communications
Centre. The Central Ambulance Communications Centre is wholly funded (100%) by
the Province of Ontario and operated under contract by the Ottawa Paramedic
Service. The funding for the Central
Ambulance Communications Centre (CACC) is separate and distinct from other
funding for the operation of the Ottawa Paramedic Service.
CONCLUSION
CONSULTATION
As this is an
administrative report, no public consultation was required.
FINANCIAL
IMPLICATIONS
The Draft 2008
Operating and Capital Budgets will include the expenditure/revenue increases
identified by this report for the 38 paramedic FTEs.
STRATEGIC
DIRECTIONS
Response time targets were developed for the City of
Ottawa in April 2002 (ACS2002-EPS-EMS-0001) taking into account international
industry standards, medical appropriateness, and community expectations. The performance targets are set at 8 minutes
59 seconds 90% of the time for life threatening calls in Ottawa’s high-density
area and set at 15 minutes 59 seconds 90% of the time for life threatening
calls in Ottawa’s low-density area[5]. Council approved these response time
targets, however, growth in the City and specifically in call volume since
amalgamation makes further investment necessary. Currently the City receives funding from the province at 50% and
the City should maximize the opportunity to access the provincial funding to
address growth per the strategic direction to “[d]eliver agreed-to level of
service at the lowest possible cost”.
DISPOSITION
The Ottawa
Paramedic Service will report back in 2008 with 2007 year-end results as well
as performance trends for the first six months of 2008.