This report outlines a Framework for the
provision of an affordable Supportive Housing Program for seniors living on low
or modest income in the City of Ottawa.
The development of the Framework was guided by a working group of
stakeholders convened by the United Way/Centraide Ottawa and led by the United
Way/Centraide Ottawa’s Seniors Impact Council.
The Impact Council’s goal was to develop strategies that would
ultimately influence a significant investment of resources by the Champlain
Local Health Integration Network (LHIN), the City of Ottawa and the Ministry of
Health and Long Term Care (MOHLTC).
Stated
simply, supportive housing in this Framework refers to any kind of housing and
support arrangement that covers the gaps between housing for completely
independent seniors and those living in long term care.
The Framework describes the key components
of an affordable and effective Supportive Housing Program for seniors including
appropriate housing, home support services, professional (health) services, the
elements of a “senior friendly” community, the importance of technology and
design, and strategies that will help sustain the program, protect the rights
and address the needs of French language seniors, and recognize the growing
diversity and overall cultural richness of Ottawa’s growing senior
population. The Framework also provides
figures on the needs of low income seniors in Ottawa that will help guide the
Program’s implementation.
The
report proposes the following five strategies to move the Supportive Housing
Program for low and modest income seniors forward:
Strategy
1: Promote Supportive Housing to
Stakeholders (seniors, caregivers, service providers, developers, politicians,
funders etc.) by:
- Developing a Vision for the Supportive Housing Program that
incorporates some of the key themes heard at the May 15th Affordable
Supportive Housing Symposium, where local stakeholders came together with
a common interest in seniors, housing and support services to help develop an action plan. For a
more detailed description of the symposium see Appendix B, page 58. (affordable, accessible, inclusive, flexible, choice,
integrated, promotes autonomy, responsive).
- Developing a communication plan that recognizes the different
target audiences (stakeholders) and strategies needed to raise awareness
about supportive housing and promote the benefits of supportive housing
and the proposed models.
- Identifying Champions in the community with credibility and
recognition to help spread the message through various public channels. An ideal champion will have
comprehensive knowledge of the issues affecting seniors and be in a
position to motivate and mobilize community, governments and businesses to
action.
Strategy
2: Add 1,400-2,000 units of supportive housing to address the needs of seniors
on low income (<$20,000) over the next five years by:
- Building on existing components of Supportive Housing in Ottawa
including the current “Aging in Place” Pilot Projects.
- Targeting neighbourhoods with high concentrations of low income
seniors such as Vanier and Centretown/Dalhousie.
- Working with supportive housing providers such as
Cornerstone/LePilier and other members of the Alliance to End Homelessness
to meet the needs of homeless seniors and those at risk of homelessness.
- Exploring new models of supportive housing such as Peel Senior
Link’s coordinated and integrated 24/7 care model and Vancouver Coastal
Health clustered care model of supportive housing.
- Supporting the recommendations of the Ottawa Alternative Level
of Care (ALC) Strategic Committee to help alleviate the pressures faced by
the hospital and long term care sector.
- Exploring with the Champlain Dementia Care Network the
supportive housing model most needed in Ottawa to assist low and modest
income seniors with dementia.
Strategy
3: Develop Partnerships and Alliances Within and Across Sectors to Implement
Models of Supportive Housing by:
- Setting up appropriate working groups including a Francophone
working group to review, assess and develop one or more of the proposed
models described in Strategy 2.
- Setting up a strategic implementation committee that would
cross sectors and be responsible for: lobbying for funds to set up Pilot
projects; identifying ways to leverage existing resources; make final
feasibility related decisions; develop a business plan for funders; help
implement the model(s).
Strategy
4: Identify and target at-risk seniors in Ottawa who are in need of supportive
housing by:
- Developing a concise user-friendly screening tool for
identification of at-risk seniors by front-line people including
physicians, police, landlords, home support workers and others in the
community.
- Developing a communication and training mechanism for various
sectors on the effective application of the screening tool, process and
protocols for connecting senior at risk with help and a “train the
trainer” workbook – all part of a toolkit.
- Using GIS technology to map existing services for seniors and
overlay where seniors on low income live across the City to identify
high-risk neighbourhoods & gaps in services.
Strategy
5: Integrate Supportive Housing Initiatives into the Broader Continuum of Health
and Social Care by:
- Developing system-wide quality performance indicators.
Exploring the use of the Resident
Assessment Instrument-Home Care assessment tool (RAI-HC) so that all service
providers are using a standardized approach.
- Inviting representation from key stakeholders within the
broader system on the Supportive Housing Working Group to help establish
respective roles and partnerships in providing supportive housing,
monitoring the program, and advocating to all three levels of government
(especially housing, health and social services) for long-term funding.
Ultimately, the goal of the Affordable
Supportive Housing Framework is to provide a blueprint for the creation of a
supportive housing program for seniors on low to modest incomes. This goal
cannot be met by a singular sector. In order to assure success, the
organizations within the Working Group must work collaboratively. A strong
commitment from United Way/Centreaide Ottawa, the City of Ottawa, the Champlain
Local Integrated Health Network as well as additional community representation
and the participation of the private sector will incontestably guarantee the
success of this endeavour.
|
Anne
Aikens
North
Renfrew Long Term Care Centre
|
Jane
Alguire
Senior Wise
Services
Inc.
|
Fara Aminzadeh
Community Research, Ottawa Hospital
|
|
Inika
Anderson
Support Services, Parkinsons Society
|
Madeleine
Anderson
Aging in Place
|
Ray
Applebaum
Peels Senior Link
|
|
Linda Assad-Butcher
LHIN Board Member
|
Bev
Bakka
UW/CO
|
Sheila Bauer
Ottawa
CCAC
|
|
Donna Berger
CCAC, Cornwall
|
Marthe
Bergevin
Association
pour l’intégration sociale d’Ottawa
|
Lucille
Berlinguette-Saumure
City of Ottawa
|
|
Christine
Bidmead
Queensway Carleton Hospital
|
Ruth Boulianne
Résidence
St-Louis
|
Robert Bourdeau
LHIN
(Champlain)
|
|
Hélène Bourgeois
South-East
Ottawa CHC
|
Dora
Brown
Interfaith Network
|
Carol
Burrows
Council on Aging of Ottawa
|
|
Ron
Campeau
CCAC, Cornwall
|
Jocelyne
Contant
Champlain LHIN
|
Tony
Cruickshank (represented by Sophie Mckeown)
Wabano Aboriginal Health Centre
|
|
Alex
Cullen
City of Ottawa
|
Kathy Danbrook
Geriatric Assessment Centre
|
John
Dickie
Eastern Ontario
Landlords Association
|
|
Christina DiTomaso
Western Ottawa Com. Res. Centre
|
Glenn Drover
ASHF Work Group
|
Paul
Durber
First United Church
|
|
Marlynne Ferguson
City of Ottawa
|
Sue Garvey
Cornerstone Housing
for Women
|
Hinda
Hassan
South-East Ottawa CHC
|
|
Kelly Hastings
Ottawa Community
Housing
|
Dennis
Jackson
Scotia Bank
|
Guirlène Jean-Baptiste
Association
pour l’Intégration Sociale
|
|
|
|
|
|
|
|
|
|
Ipshita Kamal
UW/CO
|
Barbara Lajeunesse
Forge
Com. Resource Centre
|
Johanne Levesque
Syposium
Facilitator
Ambire
SI Inc.
|
|
Al
Loney
Council on Aging
of Ottawa
|
Rosemary
Lowenger
|
Janet
Lum
Canadian Research Network for Care in
the Community
|
|
Vicki
MacKinnon
Minto
|
Louise
Martin
The Good Companions
|
Richard Mayer
Fédération
des Aînés Francophones de l’Ontario
|
|
Lee
McCarthy
Ottawa West Home Support/
Ottawa Community Support Coalition
|
Elaine
McNaughten
Personal Choice Independent Living
|
Ann Norwak
RN,BN,MEd
Ottawa Public Health
|
|
Iris
Newmann
Capital Care
|
Carmen
Perron
Veteran Affairs
Implementation Project
|
Jocelyne Pion
CSEOCS
|
|
Oris Retallack
Champlain Dementia Network
|
Lise Richard
UW/CO Ottawa
|
Jean-Louis
Schryburt
ASHF work group
|
|
Frank
Sisson
Rideau Non-Profit Housing Inc
|
Jérémy Stevenson
Senior
Planner, LHIN
|
Heather Tarnai-Feeley
Ottawa Hospital
|
|
Dennise
Taylor-Gilhen
Ottawa Parkinsons Society
|
Lise Tessier
Ottawa
Public Health
|
Shari
Westman
Comfort Keepers
|
|
Janet
Whillans
UW/CO
|
Paul
Williams
University of Toronto
|
Jim Zamprelli
Canada Mortgage and Housing
|
|
Johanne
Yelle- Weatherall
(represented by Larry Chambers)
Élisabeth Bruyère Research Institute
|
|
|
United Way Seniors Impact Council Members
Cal
Martell – Council Chair Lise Richard
Director Devlopment
Officer
Regional Geriatric Assessment Program Ottawa Community Support
Marion
Balla Carol Burrows
President Volunteer
Adlerian Counselling & Consulting Group United Way Ottawa
Sheila
Bauer Carol
Halstead
Director, Client Services Executive
Director
Champlain CCAC Township
of Osgoode
Home Support
David
Hole Jean-Louis
Schryburt
Executive Director Teacher
(retired)/Acting
South-East Ottawa centre Acting
Executive Director
for a Healthy Community ACFO,
Ottawa
Dennis Jackson Dr.
Norman Tape
District Vice-President Governor,
The Ottawa Hospital
Scotiabank-Ottawa Main Branch Federal
Government Research
Richard Mayer Marlynne
Ferguson
President Acting
Director, Long Term Care
Federation des aines et des Branch
Retraites Francophones de l’Ontario Community and
Protective Services
City of Ottawa
Diane Officer
Director, Long Term Care
City of Ottawa
Ben Franklin Place
United
Way Staff
Bev Bakka
Director, Impact and Investment
United Way Ottawa
Cal
Martell Carol
Burrows
Seniors Impact Council Chair Seniors
Impact Council
UW/CO UW/CO
Jean-Louis
Schryburt Elaine
McNaughten
Seniors Impact Council Ontario
Association of Not-for-Profit
UW/CO Homes
and Services for Seniors
Russell
Mawby Oris
Retallack
Director of Housing Champlain
Dementia Network City of Ottawa
Marlynne Ferguson Lucille Berlinguette-Saumure
Acting Director, Long Term Care Project Manager
City of Ottawa Seniors
Agenda, City of Ottawa
Jim
Zamprelli Eric
Partington
Senior Policy Researcher Senior
Consultant,
Canada Mortgage and Performance
and Contracts
Housing Corporation Champlain District
Local
Integration
Health Network (LHIN)
Jeremy
Stevenson Glenn
Drover
Senior Planner President
of Council on Aging
Champlain District Local
Integration Health Network (LHIN)
Lise
Richard Vicki
MacKinnon
Development Officer Vice President
Ottawa Community Support Coalition Special Projects, Minto
Sheila
Bauer David
Hole
Director, Client Services Executive
Director
Ottawa Community Care Access Centre South-East Ottawa Centre
for
a Healthy Community
United
Way Staff
Bev Bakka
Director, Impact and Investment
UW/CO
In early 2007, the United Way/Centraide
Ottawa Seniors’ Impact Council convened a working group of stakeholders to
develop an Affordable Supportive Housing for Seniors Framework and Action Plan
to be considered by the City of Ottawa, Ministry of Health and Long Term Care
(MOHLTC), not-for-profit housing providers and private developers. The goal of the United Way was to develop
strategies that would ultimately influence a significant investment of
resources by the Champlain Local Health Integration Network (LHIN), the City of
Ottawa and the MOHLTC.
In developing the framework, the project
team used the following approach:
- Knowledge transfer from experienced consultants hired to assist
in the development of the Framework and Action Plan;
- Literature review to identify best practices and cost effective
models of supportive housing (See Appendix A);
- Review and further analysis of secondary data sources (e.g.,
2004 Successful Aging Ottawa Seniors Survey; 2004 Ottawa Fact Book on
Aging) to help identify seniors most in need;
- Key informant interviews with other experts in supportive
housing across Canada as well as local stakeholders to identify barriers
and opportunities;
- Symposium to showcase best practices across Canada, gather
input, build consensus among local stakeholders, and explore next steps
(Agenda attached in Appendix B); and
- Meetings and ongoing discussions with members of the working
group to ensure that the Framework and Action Plan meets community
expectations.
Today the City of Ottawa is home to more
than 90,000 seniors, representing about 12% of the total population. Second
only to Calgary, Ottawa has the fastest growing senior population in Canada;
one that is projected to increase even more rapidly over the next few
decades. By 2031, the number of seniors
living in Ottawa will be triple the number of today. Such rapid growth requires
investment by governments in services for seniors. As such, it is important that the City of Ottawa be prepared with
a realistic plan that addresses both immediate needs and considers the future.
A
critical need for affordable supportive housing for seniors on low or modest
income in Ottawa has been identified in a number of recent studies:
- In August 2006 the Ottawa Alternative Level of Care (ALC) Strategic Committee released
hospital bed occupancy figures
that showed the ALC occupancy rate in acute care beds in Ottawa hospitals
is 19% and on the rise (well above other communities in Ontario). In 2004/05, Ottawa hospitals reported
46,553 ALC days, costing the system almost $25 million.
Today, there are more than 200 patients waiting in ALC, a figure that is
expected to continue to rise dramatically. The majority of these patients are seniors on low income,
waiting for placement in a basic Long Term Care room.
- Currently
in Ottawa 127 seniors are awaiting placement in long term care per 100
beds available. This situation is exacerbated by the fact that 20-25% of
seniors currently placed in LTC could be more suitably placed in
affordable supportive community-based housing. The basic cost
for a LTC bed is $132.32*/day. This compares to $550 /day for a hospital
bed and $33/day for supportive community-based care.
Note: this will increase by $1.43 as of Sept
1, 2007
- Current planning
through the Champlain LHIN predicts the need for more than 1,100
supportive housing units to be developed over the next five years.
- A recent City of Ottawa report (Seniors Agenda: 2005
Stakeholder Consultation Report) identified affordable housing including
assisting seniors to age in place as a top priority.
- In the 2004 Successful Aging Ottawa (SAO) Seniors Survey, only
26% of respondents agreed that there were enough affordable housing
options for seniors; 56% were concerned that there were not enough home
support services for seniors staying in their own home. The survey also found that most Ottawa
seniors (80%) intended to stay in their homes and had never seriously
considered moving.
- A recent Canada Mortgage and Housing Corporation (CMHC) study
on the profile of rooming house residents in Ottawa, Montreal and Vancouver
found that “aging in place” with few supports and choices in terms of
services and design aids was the norm for older tenants.
- Cornerstone/LePilier recently identified the need for
supportive housing for older homeless women with complex needs.
(>100 women age 55+ stayed overnight in shelters according to the
City’s most recent (2005) shelter count report).
- There are currently >1000 seniors on the waiting list for
affordable housing in Ottawa.
The target population for the City of
Ottawa’s Affordable Supportive Housing for Seniors Framework is seniors on low
(<$20,000) or modest (<$30,000) income. According to the 2004 Fact Book
on Aging, 41% of seniors reported a personal income of less than $20,000 and
58% indicated incomes of less than $30,000 in 2000. Women report lower personal income levels
than men, as do Francophone seniors and those from other ethno-cultural
populations.
Looking at Census household incomes for
senior-led households presents a similar picture. The last available Census reported that 17,325 Ottawa seniors
(about one third of all senior-led households) lived in senior-led households
with less than $30,000 household income and 9,490 seniors (18% of all
senior-led households) lived in senior-led households reporting a household
income of less than $20,000.
Seniors on low or modest income are most at
risk of losing their independence and being inappropriately admitted to long
term care. This is because income is related to many other factors that can
result in the same outcome. According the 2004 Successful Aging Ottawa
(SAO) Seniors Survey, compared to Ottawa seniors in general,
seniors living in low to modest income households (% of seniors with a
household income <$30,000 versus percent of seniors in general) are more
likely to report:
- Feeling in fair or poor health (30% versus 17%)
- Being a patient overnight in a hospital, nursing home or
convalescent centre in the past 12 months (17% [22% for seniors with
income <$20,000] versus 12%)
- Needing help with activities of daily living (32% versus 23%)
- Not being able to get out as often as they would like (15%
versus 9%)
According to the SAO survey, seniors on low
or modest income were also less likely to report having their health or medical
conditions diagnosed by a health professional than seniors in general (59%
versus 66%). In terms of their profile,
seniors in this income group were more
likely to be women (74% versus 58%) who are living alone (57% versus 35%) in a
home they rent (30% versus 12%). And as
reported by the 2004 Fact Book, they are also more likely to speak French in
their home (19% versus 13%) or another language other than English (17% versus
10%).
The definition of supportive housing used
in the Framework is a broad one that includes both traditional “aging in place”
models and purpose-built or designed forms of supportive housing that also
promote aging in place. As such the
definition incorporates both CMHC’s definition of purpose-built supportive housing
and the definition put forth by the Ontario Ministry of Health and Long Term
Care that links affordable housing and services. Stated
simply, supportive housing in this Framework refers to any kind of housing and
support arrangement that covers the gaps between housing for completely
independent seniors and those living in long term care.
Exhibit 1 below graphically illustrates the
Affordable Supportive Housing for Seniors Framework. It begins with the premise
that there are many ways in which supportive housing can be created.
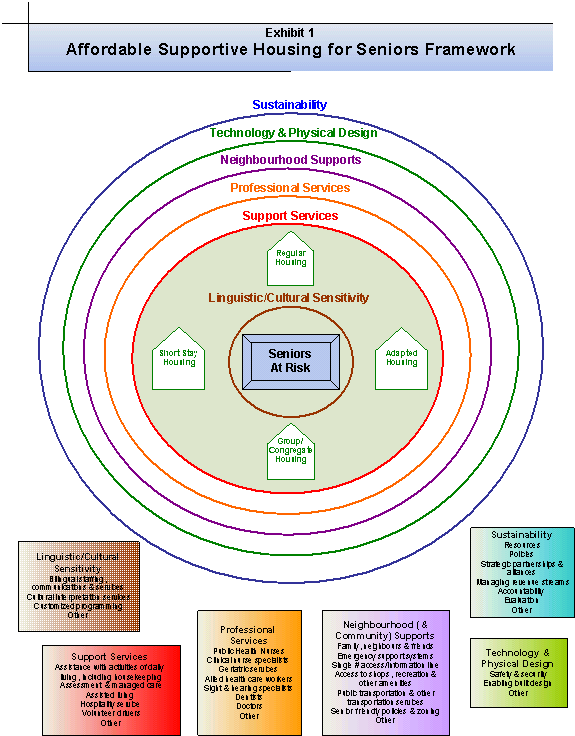
What is paramount is the appropriate
combination of supportive elements including suitably designed housing,
accessible home support services, timely professional (health) services
(including short term respite and convalescent care), and senior friendly safe
neighbourhoods and amenities created through thoughtful and inclusive city
planning policies. Underpinning the
definition is the development of a supportive housing program that offers choice
and is affordable,
sustainable, responsive, recognizes both official languages and is also
culturally sensitive to Ottawa’s diverse and multi-cultural senior population
including Aboriginal seniors, recent immigrants and gay, lesbian, bisexual and
transgendered seniors.
Supportive housing for seniors can have
many different forms. It can be created in existing private homes through a
combination of supportive services and design, or in income assisted social
housing or market rent apartments with high concentrations of seniors such as
the Aging in Place Model. Purpose-built
examples of supportive housing for seniors include small group homes such as
the Abbeyfield model (Abbeyfield Parkdale is an example in Ottawa), medium (up
to 60 units) or larger congregate settings that can stand alone or be part of a
“campus model” (such as Unitarian House in Ottawa). Assisted living facilities are included at the higher support
level under the congregate housing model. In Ottawa, assisted living is
available in some retirement homes; however, this option is currently not
affordable for seniors on low or modest income.
Supportive housing can also be provided in
mixed age communities such as mixed age market apartments, social housing or
rooming houses, by introducing initiatives and programs that encourage
neighbours and landlords to provide support. In some instances, intergenerational links can be created
by virtue of location – for example, a seniors building located close to a high school
provides the opportunity for exchange of support (seniors volunteering in
schools and vice versa).
For a more detailed description of the
different ways supportive housing can be created refer to the Literature Review
in Appendix A.
According to the 2004 SAO Seniors Survey,
23% of seniors in Ottawa need help with activities of daily living (such as
preparing meals, shopping for groceries, everyday housework, heavy chores,
personal care, and moving about). Most
seniors report getting the help they need, however, 6% of those who need help
with one or more activities of daily living say they are not receiving any
help. This percentage increases to 15%
for seniors living in households with less than $20,000 household income. Using
this percentage and projecting it to the population at large, it is estimated
that about 1,400 low-income seniors in the City of Ottawa have unmet needs and
could benefit from supportive housing (15% of 9,490 seniors living in
senior-led low-income households <$20,000). Most of these seniors live in houses they rent. (6,235 seniors
living in households with <$20,000 rent their home [66% of all low-income
senior-led households])
According to further analysis of the 2004
SAO Seniors Survey, seniors most likely to report not having the help they need
are women, over the age of 75, with little social support, and who speak a
language other than English. Although
only borderline significant,
seniors living in a rural ward were also more likely to report not receiving
any help.
The above figure (1,400) does not include
homeless seniors, seniors at risk for homelessness and seniors living in
rooming houses. This could add another
600-700 persons to the mix.
Future Projections
Projecting into the future, the number of
seniors 65+ in Ottawa (89,000 in 2001) is expected to grow to 270,000 by 2031
according to the 2004 Fact Book on Aging. This is an increase of 203%
over 30 years or roughly 7% each year – by 2010 the number of seniors will have
already increased by 70% to over 150,000.
These same projections can be applied to the numbers above.
Forms of supportive housing including aging
in place models have long been proposed by experts in gerontology and health
systems as viable options for seniors who need help with every day activities
and who without this help are at risk for losing their independence and their
choice in terms of place of residence. As well as improving the overall quality of
life of seniors, there is evidence to show that even the most basic support
service such as housekeeping can save the healthcare system money. The literature review in Appendix A provides
references to the most recent studies in this area. As well, evidence presented by the key note speaker
and others at the Affordable Supportive Housing Symposium (www.teamgrant.ca)
makes the case for a more balanced approach to health care that includes
supportive housing as an important component of the overall health system.
The key arguments in favour of supportive
housing are:
- Targeted, managed home and community care within an integrated
continuum consistently meet individual and system goals by maintaining the
health, well-being and autonomy of individuals and their caregivers and by
helping to solve key health system problems by lowering the incidence of
inappropriate use of emergency care, acute care and long term care.
- The targeted “Aging in Place” models of coordinated and managed
on-site support for high risk seniors living in income-assisted seniors
housing are cost- effective by allowing efficiencies in service delivery,
and linking seniors to appropriate services when needed.
- Lessons learned from evaluations of supportive housing for
persons at-risk of homelessness show that appropriate forms of supportive
housing are more cost- effective than the cost of no support and that
overall cost are significantly higher for institutional responses versus
community residentially based options.
This section describes the proposed
components of a Supportive Housing Program for low to modest income seniors in
Ottawa based on the Framework depicted in Exhibit 1. The components and elements described throughout this section as well
as the implementation strategies that follow focus on Ottawa. They could,
however, be applied throughout the Champlain district.
The Affordable Supportive Housing Framework
for Seniors will provide a blueprint for the creation of a supportive housing
program for seniors living on low to modest income in the City of Ottawa that
recognizes both official language groups and respects Ottawa’s diverse cultures.
The Affordable Supportive Housing Framework
for Seniors has five objectives:
- To identify a range of different combinations of affordable
housing and service supports required by seniors in Ottawa to enable them
to live as independently and as fully as possible as health and vitality
decrease;
- To draw upon evidence-based and best practices research in the
development of the Supportive Housing Program;
- To help identify critical gaps in the current mix of housing
and service supports essential to maintaining the independence and
well-being of at-risk seniors in the community;
- To help identify priorities and next steps in the short and
longer-term that will address the identified gaps; and
- To inform the Champlain Local Integrated Health Network in
their allocation decisions related to affordable supportive housing for
seniors.
The following suggested guiding principles
and prerequisites have been drawn from two sources: “best practices” described in the literature;
and a consensus of themes recorded during the small group discussions at the
May 15th Supportive Housing for Seniors Symposium – Making It
Happen.
- “Best Practices” Philosophy and Policies - Ottawa’s
Affordable Supportive Housing for Seniors Framework will:
- Target seniors most at-risk
- Foster autonomy and support independent living
- Be client-centred
- Be inclusive
- Include assessment and coordination of care and service
- Give clients access to 24-hour support
- Provide 24-hour emergency response
- Be integrated into the broader continuum of health and social
services
- Be accountable
- Be sustainable
- “Best Practices” Service Delivery - Ottawa’s Affordable
Supportive Housing for Seniors Framework will:
- Be flexible and personalized in its delivery
- Offer a variety of affordable housing and support service
models
- Employ ‘case management’ functions of case finding,
care/service coordination, referrals and community development
- Address multiple client needs (i.e., Alzheimer’s, addictions,
mental health, cultural)
- Offer flexible, consistent staffing
- Be sensitive to linguistic, multicultural and other client
diversities and needs in recruiting, hiring, training programs and
education
- Employ accessible communication tools for frontline staff
(e.g., pager, cell phone)
- “Best Practice” Administration and Management - Ottawa’s
Affordable Supportive Housing Framework for seniors will:
- Show leadership through common vision, commitment, and an
understanding of at-risk seniors’ needs and informed decisions
- Provide specialized environments for special needs (e.g.,
Alzheimer’s)
- Create efficiencies through critical mass
- Use the latest client information management software
- Hire only “people focused” staff
- Involve seniors in decisions that affect them
- Understand and communicate with family members/caregivers
- Establish realistic expectations about access and costs of
support services
- Support staff in their work
- Establish policies on the rights and responsibilities of
residents
- Evaluate the effectiveness of services including client
satisfaction
- “Best Practices” Linkages and Relationships - Ottawa’s
Affordable Supportive Housing Framework for seniors will:
- Collaborate with all housing providers for assessment,
admission, ongoing reviews, and other issues
- Enhance access and linkages to a larger range of services,
including health and long-term care
- Link with hospitals and other formal health care service
providers (e.g., physicians, clinics, outreach), other community service
groups, volunteers, local business, cultural organizations and networks
- Develop alliances with other health care agencies providing
related services in the same building
The circle diagram shown in Exhibit 1 is
meant to illustrate a non-linear and dynamic approach to a comprehensive
supportive housing program for low and modest income seniors. Each of the circles represents an important
component of the program and each component contains elements that enhance the
quality and effectiveness of the overall program. This section will briefly describe the major components and their
key elements.
In this proposed framework for Ottawa’s low
income and modest-income seniors,
at-risk seniors are positioned in the centre
of the circle diagram. The different
elements of an optimal supportive housing environment wrap around the senior as
determined by their individual requirements, circumstances and resources
available. The presence of case
managers, needs assessment and coordination would facilitate the mobilization
of the appropriate mix of resources and housing for the at-risk senior,
wherever he/she may be residing in their home, in congregate or in hospital
environments.
This circular framework also recognizes
that intensity of need for supports does not always progress in a linear
fashion towards increasingly more intensive types of supportive housing. For example, some at-risk seniors with
relatively intensive support requirements can reside comfortably and safely in
their own homes while other seniors with the same service support requirements
but different circumstances may be more appropriately supported in a 24/7
on-site congregate model of supportive housing. By putting the senior at risk in the centre of this circular
diagram, the different pathways that at-risk seniors often take based on their
individual needs and circumstances at any given time are recognized. Flexibility and choice underpinning the
overall framework will lead to responsive and cost-effective approaches for
at-risk seniors.
Central to the well-being of all seniors is
appropriate housing. For seniors on low
or modest income this is often a challenge in later life. CMHC has provided figures that show that 19%
(>10,000) of Ottawa seniors live in households that are either not
affordable (too expensive for their income), not suitable (too large or too
small) or not acceptable (too run down).
Many older people continue to reside in the
home they raised their families and as they age, their activities, household
composition and resources alter. Owners of older property face increasing
maintenance or the need to make modifications to their homes while their own
health and ability to cope with these issues is deteriorating. Older renters must deal with public and
private landlords who are less willing to make adaptations to meet the needs of
their older tenants. Increased rent can
also become a problem. Inappropriate
housing alone can sometimes be the reason why an older person on low income
goes straight into a nursing home.
There are simply not enough affordable options in between.
A supportive housing program can address
the issue of inappropriate housing by linking seniors to affordable home help
services in the community, government programs such as Residential
Rehabilitation Assistance Program (RRAP), Home Adaptations for Seniors
Independence Program (HASI), and information about alternative financing
arrangements such as reverse mortgages.
Exhibit 1 shows that supportive housing can
be provided in regular housing (as described earlier), seniors-only housing
(Aging in Place Model) or by facilitating the development of affordable
purpose-built supportive housing.
Ottawa is a bilingual city and as such
access to services in both official languages is a basic right. For seniors on low or modest income, it is more
significant. Seniors who speak French
are more likely to report living in a low income household and, as it has been
shown in the analysis detailed earlier, are also more likely to need supportive
housing.
In addition to addressing the unmet needs
of French language seniors, the supportive housing program must be sensitive to
the needs of seniors from many different backgrounds including Aboriginal
seniors, newcomers and seniors from the gay, lesbian, bisexual and
transgendered community.
Elements that will foster inclusiveness
include:
- Programs and services being offered in both official languages
- Access to cultural interpretation and translations services
where needed
- Cultural sensitivity workshops offered to staff
- Working together with existing community alliances and
collaborative groups to design appropriate programs (such as Fédération
des aînés et des retraités francophones de l’Ontario, Ottawa-Carleton
Immigration Services Organization, Native Friendship Centres, Odawa, Pink
Triangle Association, Wabano Aboriginal Community Health Centre etc.)
Ottawa offers a range of community support
service to seniors through the Champlain Community Care Access Centre, the
Ottawa Community Support Coalition, Community Resource Centres, and Community
Health Centres etc. The types of supportive services that have been shown to
most benefit seniors and foster independence include:
- Help with activities of daily living such as shopping,
housekeeping, banking, telephoning, meals
- Transportation (volunteer drivers, specialized transportation)
- Escort to appointments
- Assessment and managed care
- Help with personal care such as dressing, bathing and toileting
(assisted living)
- Help with medications (assisted living)
- Palliative care (assisted living)
A number of studies (Lum et al, 2005;
Hollander, 2006) have pointed to the importance of integrating the services
around the needs of the client. It has also been found that the provision of
lower cost services such as housekeeping can have a significant impact on the
cost-effectiveness of a health care system.
Currently services are arranged and
delivered in several ways:
- Residents can receive services in their home directly from
community agencies on a pay as you go basis
- In purpose-built supportive housing, services are typically
offered as part of the resident’s monthly accommodation fee
- Residents in some purpose built supportive housing can also use
services on a pay as you go basis, at a monthly or yearly fee
Panel members at the Supportive Housing
Symposium on May 15th introduced some interesting delivery
approaches including the Clustered Model in Vancouver where the delivery of
services is clustered either in a building or neighbourhood to provide greater
continuity of care and to achieve greater efficiencies (link to presentation on
the web site). Peel Senior Link offers
24/7 on-site support to seniors in social housing through an integrated service
model that targets residents most at risk
(http://www.peelseniorlink.com/).
Whatever the arrangement of service
delivery, the most critical gap for aging in place at home for low to modest
income seniors is a publicly funded program that would provide housekeeping and
homemaking services on a long-term basis
– similar to the Integrated Homemaker Program that was discontinued
in the mid-‘90s.
The framework recognizes the importance of
linking the at-risk senior to responsive and knowledgeable (about seniors)
professional services including:
- General practitioners that are aware of what is available in
the way of community supports for their older patients
- Geriatric services
- Timely access to specialists
- Clinical nurse specialists
- Allied health care workers
- Sight and hearing specialists
- Footcare clinics
- Dentists
For those connected with the agencies that
provide supports available in the community, referral to these professional
resources likely occurs. However,
research has indicated that the at-risk senior is more likely than not to be isolated,
without family and friends to advocate on their behalf. Some at-risk seniors may only have contact
with their family doctors, but unless doctors are aware of the resources
available and help the senior to make the necessary connections, the at-risk
senior is unlikely to access these vital professional services.
Exhibit 1 acknowledges that family, friends
and neighbours are an important source of support for many seniors. In fact,
research has shown that supporting caregivers may also save the system
money. Indeed, in the 2004 SAO Seniors
Survey, 92% of respondents reported that they had someone to turn to when they
needed help with things like meals, rides or chores. And just over 40% referred
to family or friends when they needed medical advice.
A supportive community can also be created
through thoughtful City planning, policies and programs. Some key elements of a “senior-friendly”
supportive community include:
- Accessible public transportation in terms of design (easy
step-up), routes, hours of operation, driver education (about seniors)
- Policies and zoning flexibility that allows the creation of new
supportive housing such as secondary suites, granny flats, purpose-built
congregate housing
- Emergency and safety support systems such as 911, personal
emergency response systems linked to neighbourhood response centre,
neighbourhood security check systems (i.e., Neighbourhood Watch), traffic
safety programs and refresher courses
- Universal community design that includes improved street
lighting, additional benches, well-maintained streets and sidewalks (snow
and ice clearing in the winter), flat curbs for scooters and walkers,
increased signage, more time to cross the street etc.
- Single access number/information line for seniors services
- Affordable recreational and social activities
- Affordable educational and cultural opportunities
According to a recent report by Canada’s
Public Health Agency, between 25% and 75% of falls by older people involve an
environmental component including stairs and other factors in and around the
home. Almost 62% of injury-related
hospitalizations for seniors are the results of falls. Reducing the incidence of falls among
seniors would most certainly save healthcare costs. Home modifications should be an important component of a falls
prevention program. According to the
2004 SAO Seniors Survey, only 38% of respondents reported having grab bars in
their bathroom, considered a minimum basic home modification – other supportive
design features were less common.
Advances in technology and good design can
go a long way in the provision of a safe and supportive environment for
seniors. Application of appropriate
technology and design can:
- Keep a home safe
- Enable the senior to function independently; i.e., carry out
activities of daily living (instrumental and self care)
- Provide efficiencies in operations (e.g., zero entry shower
allows the frail senior to bathe without assistance and minimizes risks
such as falls)
- Design can facilitate social interaction
- Increase sense of safety and security
- Promote independence and continued engagement in the community
(e.g., walkers, canes and wheelchairs promote freedom of movement)
- Facilitate communication (e.g., hearing aids, telephone handset
with built-in volume, flashing signals for door bells, etc.)
- Increase vision (sunglasses, large playing cards, touch tone
phones, magnifying glasses etc.)
- Increase coping skills (e.g., memory aides such as writing
lists, using pictures to label contents, using pill organizers, talking
clocks, and vibrating phones etc.)
Canada’s Public Health Agency has recently
published a guide to home safety for seniors available at the following
website: http://www.phac-aspc.gc.ca/seniors-aines/pubs/safelive/index.htm. CMHC offers a program, Home Adaptation for
Seniors Independence (HASI) that assists seniors on low income to make small
changes to their home to help them stay longer than would otherwise be
possible. CMHC has produced a number of
recent publications related to purpose-built supportive housing for
seniors. In addition, CMHC’s Rental Residential
Rehabilitation Program (Rental RRAP) offers financial assistance to landlords
of affordable housing to pay for mandatory repairs to self-contained units
occupied by low-income tenants. Mandatory repairs are those required to bring
properties up to minimum levels of health and safety. More information on the
enabling role of technology and design and available resources is contained in
Appendix C.
Providing affordable supportive housing
that is also sustainable over the long run is challenging and will require new
resources as well as innovative approaches.
Strategies that will help include:
- Developing strategic partnerships and alliances including
private/public partnerships (e.g. Minto) to leverage resources, share
market intelligence, coordinate efforts etc.
- Linking to City of Ottawa Housing Strategy and City of Ottawa
Rooming House Strategic Planning Framework to explore common goals and
strategies (e.g. advocacy to different levels of government)
- Managing revenue streams which are expected to come from
multiple sources
- Accessing CMHC programs and
financial assistance such as Homeowner RRAP, Disabled RRAP, Secondary
Suites RRAP and HASI described at
www.cmhc-schl.gc.ca/en/co/prfinas/index.cfm
- Being accountable by developing realistic performance
indicators and benchmarks
- Evaluation to demonstrate impact of model on clients and the
system
The
following five strategies and associated actions are proposed to move the
Supportive Housing Program for low and modest income seniors forward.
Strategy
1: Promote Supportive Housing for
Seniors to Stakeholders (seniors, caregivers, service providers, developers,
politicians, funders etc.) by:
- Developing a Vision for the Supportive Housing Program for
Seniors that incorporates some of the key themes heard at the Symposium
(affordable, accessible, inclusive, flexible, choice, integrated, promotes
autonomy, responsive etc.).
- Developing a communication plan that recognizes the different
target audiences (stakeholders) and strategies needed to raise awareness
about supportive housing and promote the benefits of supportive housing
and the proposed models.
- Identifying Champions in the community with credibility and
recognition to help spread the message through various public channels.
Strategy
2: Add 1400-2000 units of supportive housing to address the needs of seniors on
low income (<$20,000) over the next five years by:
- Building on existing components of Supportive Housing in Ottawa
including the current “Aging in Place” Pilot Projects.
- Targeting neighbourhoods with high concentrations of low income
seniors including those living in rooming houses such as Vanier and
Centretown/Dalhousie.
- Working with supportive housing providers such as
Cornerstone/LePilier and other members of the Alliance to End Homelessness
to meet the needs of homeless seniors and those at risk of homelessness.
- Exploring new models of supportive housing such as Peel Senior
Link’s coordinated and integrated 24/7 care model, Vancouver Coastal
Health clustered care model of supportive housing, and Deep River’s rural
model of Long Term Care. (For a description of two other promising models
see Appendix D)
- Supporting the recommendations of the Ottawa Alternative Level
of Care (ALC) Strategic Committee to help alleviate the pressures faced by
the hospital and long term care sector.
- Exploring with the Champlain Dementia Care Network the
supportive housing model most needed in Ottawa to assist low and modest
income seniors with dementia.
Strategy
3: Develop Partnerships and Alliances Within and Across Sectors to Implement
Models of Supportive Housing by:
- Setting up appropriate working groups including a Francophone
working group to review, assess and develop one or more of the proposed
models described in Strategy 2.
- Setting up a strategic implementation committee that would
cross sectors and be responsible for: lobbying for funds to set up Pilot
projects; identifying ways to leverage existing resources; make final
feasibility related decisions; develop a business plan for funders; help
implement the model(s).
Strategy
4: Identify and target at-risk seniors in Ottawa who are in need of supportive
housing by:
- Developing a concise user-friendly screening tool for
identification of at-risk seniors by front-line people including
physicians, police, landlords, home support workers and others in the community.
- Developing a communication and training mechanism for various
sectors on the effective application of the screening tool, process and
protocols for connecting senior at risk with help and a “train the
trainer” workbook – all part of a toolkit.
- Using GIS technology to map existing services for seniors and
overlay where seniors on low income live across the City to identify
high-risk neighbourhoods & gaps in services.
Strategy
5: Integrate Supportive Housing Initiatives into the Broader Continuum of
Health and Social Care by:
- Developing system-wide quality performance indicators.
- Exploring the use of the Resident Assessment Instrument-Home
Care assessment tool (RAI-HC) so that all service providers are using a
standardized approach.
- Inviting representation from key stakeholders within the
broader system on the Supportive Housing Working Group to help establish
respective roles and partnerships in providing supportive housing,
monitoring the program, and advocating to all three levels of government
(especially housing, health and social services) for long-term funding.
A. Paul Williams, Professor, University of
Toronto, Supporting Seniors & Sustaining Medicare: Supportive Housing in
the Balance of Care. Presentation, Ottawa Supportive Housing for Seniors
Symposium: Making it Happen, May 15, 2007.
Alternative to Appropriate Levels of Care:
Ottawa ALC Strategic Committee Report of Recommendations, August 2006.
Canada Mortgage and Housing Corporation,
Profile of Rooming House Residents. Research Report Prepared by Social Data
Research Ltd., May 2006.
Canada
Mortgage and Housing Corporation, Life Lease Supportive Housing: Combining the
Best of Housing and Complex Care. Prepared by The Capital Care Group, February
2005.
Canada
Mortgage and Housing Corporation , Life Lease Housing in Canada: A Preliminary
Exploration of Some Consumer Protection Issues. Prepared by Lumina Services
Inc., June 2003.
Canada Mortgage and Housing Corporation,
Supportive Housing for Seniors. Research Report Prepared by Social Data
Research Ltd., 2000.
Connecticut Supportive Housing
Demonstration Program. New Haven Corporation for Supportive Housing,
www.csh.org.
Evaluation of the Aging in Place Pilot
Project: Final Report. Prepared by The Flett Consulting Group Inc. & Social
Data Research Ltd., 1996.
Flett, Darlene E., Last, John M.,
&Lynch, George: Evaluation of the
Public Health Nurse As Primary Health-Care Provider For Elderly People. Aging
in Canada – Social Perspectives, edited by Victor W. Marshal, Fitzhenry &
Whiteside, 1980.
Hollander Analytical Services Ltd.
Literature Review on the Cost-Effectiveness of Continuing Care Services.
Veteran Affairs Canada and the Government of Ontario, July 2006, www.hollanderanalytical.com
Lum, Janet M., Simonne Ruff & A. Paul
Williams, When Home is Community: Community Support Services and the Well-Being
of Seniors in Supportive and Social Housing. United Way of Greater Toronto,
April 2005.
Mancer,
Kate and Carole Holmes, 70 Ways to Reduce the Cost of Developing and Operating
Supportive Housing for Seniors. Funded by the Real Estate Foundation of BC for
the BC NON-Profit Housing Association, October 2004.
National Advisory Council on Aging, The
NACA Position on Supportive Housing for Seniors: No. 22, October 2002.
Ontario Seniors Participation in Health
& Housing Policy: Summary of Main Issues. Prepared by the Ontario Coalition
of Senior Citizens Organizations for Health Canada, January, 2003.
Pomeroy, S., Focus Consulting, Proactive
Versus Reactive Responses to Homelessness: A Costing Analysis. Paper Presented
to the Alliance to End Homelessness Community Forum on Homelessness. November
22, 2006.
Social
Data Research Ltd., Searchable Database of Supportive Housing for Seniors in
Canada. Prepared for Health Canada, April 2005. http://www.hc-sc.gc.ca/hcs-sss/pubs/care-soins/2005-seniors-aines/index_e.html
The Council on Aging of Ottawa, 2004 Fact
Book on Aging: Seniors in the New Ottawa.
Vancouver Coastal Health, Outcome
Evaluation: Changes in Hospital Utilization by Individuals One Year Post Access
to Supported and Non-Supported Affordable Housing. Vancouver, British Columbia,
October, 2006 (For more information contact Linda Thomas, Director, Housing
Services, Linda.Thomas@vch.ca)
The purpose of this literature review is to
provide relevant and recent background information about supportive housing for
seniors including:
- A definition of supportive housing
including the major elements
- The relationship between supportive
housing, aging in place and healthy aging
- A profile of seniors who could
benefit from supportive housing
- The different types of models of
supportive housing and cost effectiveness
- Best practices and innovative
initiatives
An internet scan, keyword search of the
academic literature and correspondence with experts in aging was used to
identify relevant articles and reports referred to in this review. The review
was international in scope.
To date there is no consistent definition
of supportive housing in Canada. In fact, the definition of supportive housing
varies across jurisdictions, both within Canada, and internationally. Although
there may still be no accepted "official" definition, a good
"working" definition of supportive housing in Canada has been
provided by Canada Mortgage and Housing Corporation (CMHC):
“Supportive housing is a term used to describe a range of housing
options designed to accommodate the needs of seniors through design
features, housing management, and access to support services. At one end of the range, supportive housing
refers to congregate housing with supportive features and services such as
monitoring and emergency response, meals, housekeeping, laundry and
recreational activities. At the other
end of the range (referred to in most North American jurisdictions as “assisted
living”) personal care services are also provided for frailer seniors with more
significant support needs. Professional services may be provided on a home-care
basis in a supportive housing setting as they would be if the resident were
living in a different kind of (non-supportive) residential setting. Supportive
housing may be provided by either the public or the private sector, for profit
or not for profit. In some cases, one
provider will be responsible for delivering the whole supportive housing
package (services plus housing). In other cases services and housing components
will be delivered separately, by different sectors. Supportive housing can be
rented, purchased as a condominium in fee simple, or obtained through a life
lease.”
According to CMHC, “supportive housing is
currently being developed to provide Canadian seniors with an intermediate
housing alternative, between living alone without supports (staying at home)
and the heavily regulated environment of institutional care”. For simplicity, supportive housing is
“housing with services for seniors regardless of government involvement and
independent of any specific government program referring to “supportive
housing” in its title or description.
According to
CMHC’s definition, for housing to be supportive it must have the following five
key components: First, supportive housing should have a
home-like, residential character – in other words not be institutional. Second,
supportive housing should be physically supportive – an environment in which
residents and visitors can move about freely and have access to common areas
for active living and socializing both indoors and outdoors. Third, supportive
housing should facilitate access to necessary support services for assistance
with activities of daily living. Fourth, supportive housing and service
providers should have a progressive management philosophy that is “people
focused” and allows for good communication between providers and residents. And
fifth, seniors should have access to supportive housing that is affordable and
offers choice in terms of services offered, tenure and types of residents.
In 2005, Social
Data Research Ltd. (SDR) collected information from 244 supportive housing
providers across Canada as part of a two year pilot project to develop an
inventory of seniors supportive housing and a searchable database. CMHC’s definition of supportive housing was
used to help define the survey parameters. The survey was restricted to
projects that had been purpose built or converted to supportive housing in the
last fifteen years.
The survey
presented a snapshot of projects that currently exit in Canada and the
residents who live in these projects.
Most projects were located in Quebec, Alberta, Ontario and British
Columbia. About half the projects
opened in the last ten years. About
one third of the operators defined their projects as assisted living. The
survey identified projects from all sectors:
public, private non-profit and private for-profit. They ranged in size from as small as less
than ten units to as large as 400 units. One-bedroom suites appear to be the most prevalent although many
projects offer more than one size of unit.
Almost all (99%)
of projects offer some services on site through their own organization. The majority of projects offer: 24-hour
security; unit repairs/maintenance; meals served in a common dining room;
recreational activities; hospitality services such as personal laundry and housekeeping;
help with medications; and assistance with activities of daily living. Some projects also offer: transportation
assistance (such as a facility-dedicated van); escorts to appointments; doctor
visits; social services (such as counseling and referrals); mental health
services; meals on wheels or wheels to meals; and palliative care.
The majority of projects have an on-site service coordinator who helps
residents to access services. Most projects also involve residents in
management decisions that affect them.
About half the projects have on-site staff. In some projects residents
and front-line staff are asked to sit on advisory boards or are involved in
some other capacity related to management.
Projects were
asked to provide information on the minimum and maximum monthly cost of housing
and support services to their residents.
About 70% of respondents provided information on costs. The average minimum cost to residents
reported was $866 per month, and the average maximum cost was $1,264. However,
reported rates for some projects were as high as $4,200 per month. Almost all projects offered a subsidy to
residents who could not afford the full costs.
According to the
2005 SDR survey of supportive housing projects for seniors across Canada, the
average age of residents living in supportive housing ranges from 63 to as old
as 93. Most are women, and almost all
are living alone. Residents of supportive housing come from many different
cultural backgrounds, and some projects are sponsored by a particular ethnic or
religious organization.
About 70% of the
projects in the survey reported they have been designed to support “aging in
place”. As a result some residents are quite frail and need help with most
activities of daily living. However, on average, about half the residents
require little or no assistance and function quite independently. Many supportive housing projects have some
residents with dementia; however, very few have been purposely designed to
serve the needs of persons with dementia.
The 2005 SDR
survey also included a literature review and interviews with experts in
supportive housing across Canada. One of the themes that arose in the review
centered on the issue of where supportive housing fits in the continuum of
housing and care for seniors with greater health needs. For persons who do not require 24-hour
nursing care, experts agree that most forms of supportive housing make it possible
for residents to safely “age in place”.
However, for seniors with severe dementia or other chronic diseases that
result in significant loss of abilities over time, supportive housing may not
be able to sustain these individuals over the longer term.
Although most projects in the survey reported that they have features that
support aging in place, only 16% indicated that they have been designed to
serve the needs of persons with dementia.
As well, 54% restrict tenure for persons with mental health issues such
as dementia.
The standards of
care (or lack of standards) and how this relates to the quality of life for
residents in supportive housing are still hotly debated. To help maintain a
high level of quality of life in supportive housing, some experts hold the view
that clear provincial policy guidelines related to standards and quality of
services are needed. However, at the
same time, concern is expressed about setting standards that are too
restrictive.
At the time of the
SDR study (still true today), BC was the only province with any legislation in
place related to supportive housing.
Current legislation in BC restricts assisted living facilities in BC to
providing mainly hospitality type services and only one or two of the
prescribed higher forms of more intensive services.
To be eligible for assisted living in BC, all persons must be assessed by the
regional health authority as needing the level of care provided by assisted
living facilities. The BC legislation specifically excludes people “who are
unable to make decisions on their own behalf” from private and public assisted
living unless they reside with a spouse who is able to make those decisions for
them.”
The lack of
national standards for supportive housing and differing access criteria for
home support services across the country are seen as barriers to the
development of good quality supportive housing for seniors. Since the SDR
report, CMHC released
a report that outlines a legal framework for supportive housing for seniors
that could help policy makers explore regulatory options. (Described under Best
Practices in this Report).
A few years ago
CMHC conducted a fairly comprehensive study of resident satisfaction in
supportive housing. To date, it still remains the only study of
its kind. The researchers conducted 24
case studies of supportive housing options for seniors across Canada and
interviewed more than 500 residents.
They examined resident satisfaction in detail across several major
areas: housing features (private and common spaces), tenure arrangements,
social involvement and interaction, management and operational approaches,
support services, amenities and overall satisfaction.
Overall, the User
Satisfaction study found a high level of resident satisfaction with most
aspects of supportive housing, however, some projects were rated more highly
than others. It was difficult to
discern which factors distinguished those providers who received a high rating
and those who did not because the study was presented in a descriptive manner
and did not draw any conclusions. The research did seem to show that the
provision of a range of responsive support services was important to
residents. Projects that were successful
in this regard were rated more highly.
Staffing and
family support are important issues related to the quality of supportive
housing and ultimately resident satisfaction and quality of life. A recent study compared three different
types of settings in Alberta – adult family living, assisted living, and
dementia care residential settings. Recall and stylized time-use methods were used to assess the types
of tasks and amounts of service provided by family and staff caregivers in the
three settings. The study found that
family members provide about 30% of on-site services to residents. Family members spend most time in enhancing
well-being, while staff spends most time in housework. Patterns of care differed across the three
settings. Family members of residents in assisted living residences tended to
spend more time providing care than those in the other two settings. Given the
major involvement of family members in service provision, the researchers
recommended that future program policies and practices recognize this
involvement and its impact on family caregivers.
Outside of the CMHC definition which
restricts supportive housing to purpose built or modified congregate housing,
others provide a broader range of different supportive housing models. The list below describes this broader range
and the types of seniors that would most benefit from each of these models.
- Existing private homes that are adapted to produce a more supportive
environment in an individual's own home through a combination of
physical design changes, bringing companionship by sharing the home with
another person (or persons) and accessing community support services. This type of supportive housing is
ideal for a “house poor” senior living alone (or with their spouse) in a
larger home that is owned who needs some security and companionship, extra
income from rent, and a little help with home maintenance. “The golden girls” model is a form of
home sharing where two or more seniors (typically women) decide to share a
home – sharing costs and providing mutual support.
- Supportive
housing can also be created in an existing home by adding on an accessory apartment, secondary suite or
a garden suite/granny flat – a small separate home that is built on the
property of the "host" home.
This type of supportive housing works well for those adult children
and their parents (typically a widowed mother) who get along and are able
to negotiate an arrangement openly and realistically. Children must be prepared to provide
support and to help facilitate access to community support services when
needed.
·
Abbeyfield houses are small group homes that were initially designed in
Great Britain for elderly, unattached people and those who are socially
isolated and at risk of self-neglect.
There is usually a housekeeper onsite who prepares meals, carries out
housework and shopping. This type of supportive housing is for seniors who need
more supervision and support than those relying on family and tenants for
assistance. It is not suitable for seniors who need extensive personal care or
whose behaviours are socially unacceptable.
·
Congregate housing is a purpose built or modified form of supportive housing
typically offered by the private sector.
This type of supportive housing can range from a smaller development of
forty units or less to larger ones of 100 units or more. Most developments offer one or more meals
per day, emergency assistance (though medical staff are typically not on-site)
and some level of support services, sometimes with options. “Assisted living” facilities are included at
the higher support level under this category.
Imported from the US, assisted level facilities (more common in Alberta
and British Columbia) offer 24 hour staffing, personal care, meals and snacks,
housekeeping, laundry and maintenance services. In congregate housing seniors live in private, self-contained
suites which are lockable. Suites vary in size from bachelor suites to one or
two bedroom apartments. This type of
supportive housing is suitable for a wide range of seniors since it usually
provides a mix of privately and publicly funded support services. A large
enough complex can accommodate more diverse personalities and needs than a
small place like an Abbeyfield house.
At the assisted living end of the continuum, seniors with mild or medium
dementia can often be accommodated although there is some debate in the
literature about this issue. Most assisted living facilities have been
developed by the private sector and target a more affluent senior.
·
The campus model of supportive housing
provides a multi-level of care for residents so that they can “age in place” as
their health needs change. The campus
model typically has a combination of independent apartments for seniors, congregate
supportive housing for frail elderly persons, and nursing care, on-site (i.e.
assisted living) so that a continuum of care can be provided to residents. This model can accommodate seniors with no
need for assistance, to those who just need to be provided with meals, to those
who need nursing care. In addition to
individuals being able to age in place, another advantage is that spouses with
different levels of care needs can live in the same complex.
·
Other creative
models include cohousing/collaborative
housing (mixed generational housing) and satellite homes. In a cohousing
development residents usually own their individual homes, which are clustered
around a "common house" with shared amenities. These amenities may
include a kitchen and dining room, children's playroom, workshops, guest rooms,
home office support, arts and crafts area, laundry and more. Each home is
self-sufficient with a complete kitchen, but resident-cooked dinners are often
available at the common house for those who wish to participate. Satellite
homes are group homes or “cottages” designed for seniors who can live in a
group situation who need personal or intermediate care. The “host” organization which can be a long
term care facility, church, or seniors support services organization provides
the staffing and necessary care.
There are a variety of tenure arrangements in supportive
housing including: subsidized rental, market rental, condominium, equity co-ops
and life leases. Each of these forms of
tenure impact affordability in different ways and lack of awareness about a
particular type of tenure form can become a barrier to the development
process. Life Lease for example, is a
form of tenure that has had mixed successes depending on the sponsor and yet
has a great deal of potential in terms of facilitating aging in place.
An interesting supportive housing model has been developed
in Edmonton, Alberta but can be found in other provinces. This model has been
described as a “careaminium”. It is a
setting in which people purchase a condominium on a life lease. The home can be
a one or two bedroom unit. The
condominium developer, a long term care facility operator, provides all needed
services. This model allows couples to
live together in the same unit even when one partner needs a higher level of
care than the other (unlike in the campus model or continuum of care model
where spouses become separated).
Ontario’s supportive housing
program was born out of research conducted during the eighties that showed a
need for support services for low-income seniors and families living in social
housing. A provincial supportive
housing program was introduced that provided additional funding for support
programs in selected communities across the province that were considered
“under-serviced” in this area. Today,
supportive housing buildings are owned and operated by municipal governments or
not-for-profit groups. Accommodations,
on-site services, costs and the availability of subsidies vary with each
building. The housing portion of
supportive housing is rental accommodation covered by the Tenant Protection
Act, 1997. The Ministry of Health and Long-Term Care funds personal care and
support services costs.
In the City of Toronto a range of supportive housing models
is described along a continuum of independence ranging
from:
·
Low
Support High Rise Model where residents live in
self-contained units in an apartment building with or without on-site support
services (greatest independence) and may have access to services offered by a
nearby congregate housing facility.
·
Low
Support Congregate Model where residents have
access to the same support services as above but do not live in totally
self-contained units but rather share common dining facilities and other
services. This model can successfully house vulnerable seniors who also have
significant mental health problems. (e.g., LOFT/John Gibson House)
·
Medium
Support Multi-Service Model where residents live in
a housing complex that is very close or attached to a multi-service agency and
has easy access to other services that are operated on the larger site (e.g.,
elderly person’s centre, medical clinics, restaurants etc.). This model
minimizes social isolation because of the proximity to support staff. Some
seniors may be able to age in place longer than in less supportive models.
·
Medium+Support
Horizontal and Vertical Campus Models where seniors
live in a congregate setting that is either nearby (horizontal) or part of
(vertical) a long term care centre. In both cases residents have access to the
full range of personal and nursing services needed for more complex care. The Baycrest Centre is a good example of
this model and also includes a geriatric hospital.
·
High
Support Specialized Model where residents live in a
closely monitored, specially designed physical environment for seniors with
special needs. (least independence):
Assisted living facilities (ALFs) are a residential model
of care that have received considerable attention in the US as a potentially
less expensive and more appealing alternative to nursing homes. ALFs are now commonly found in Canada mainly
in Alberta and British Columbia but also elsewhere. The Assisted Living Quality
Coalition has defined assisted living as a congregate residential setting that
provides or coordinates personal services, 24 hour supervision and assistance
(scheduled and unscheduled), activities and health related services and is
designed to minimize the need to move; to accommodate individual residents’
changing needs and preferences; to maximize residents’ dignity, autonomy,
privacy, independence, and safety; and to encourage family and community
involvement.
Services and staffing can be arranged in a number of ways
and are typically provided through partnerships between housing and service
providers. Hollander, in his recent
literature review
described three types of assisted living partnership models:
·
The
Informal Model – in this model the assisted living
provider hires its own staff for private-pay health monitoring. The home care
agency simply provides one-to-one care for clients who live in the assisted
living building. There are no written
agreements or partnerships between the assisted living provider and home care.
This is the common model.
·
The
Preferred Provider Model – In this model the
assisted living provider still hires its own staff but enters into a letter of
agreement with one or more home care agencies to serve as “preferred providers”
of home care services.
·
The
Comprehensive Model – In this model there is a
formal contract between the assisted living provider and the home care provider
to have the home care agency provide the full range of private-pay personal
care and health monitoring for all residents, and government subsidized home
care services.
Supportive
housing is often used in parallel with the concept “Aging in place”. In reality, the latter can actually be an
outcome of the former. Aging in place,
commonly means not having to move from one’s present residence in order to
secure necessary support services in response to changing needs. It also assumes that most seniors prefer to
remain in their home and indeed consumer research suggests that this true. The
2004 Successful Aging Ottawa Survey found that only 20% of seniors had
seriously considered moving from their current home in the past year in spite
of factors such as the home being too large and difficult to maintain,
cost/financial reasons or health reasons.
In fact, according to Statistics Canada, seniors made up only a small
fraction of movers between the years of 1999 and 2001 in contrast to people
under the age of 65. Seniors who rent are more likely to have moved than
seniors who own their home.
Aging in
place may not be a positive experience for all seniors. A recent British paper
questions this notion for vulnerable seniors.
The author contends that factors such as house disrepair, homelessness
and thoughtless or unresponsive landlords can undermine a persons “quiet
enjoyment” of home. In drawing
conclusions, the author considered international perspectives on aging in place
and found many similarities and common trends.
The author reported that the policy focus in most countries is shifting
away from institutional care towards supporting frail older people in their
homes through the provision of health and social care services. However, many seniors fall through the
cracks particularly those living in unstable housing situations including the
homeless and persons with dementia.
As such
the bottom line for many older people is not that they are vulnerable per se
but that they live in vulnerable housing situations. The British paper
concludes that there is a need for policy makers to respond to the diversity of
circumstances in later life and that this response needs to address housing
issues explicitly. “Aging in place” and
“staying put” are viewed as slogans that could be turned into reality by
denying access to more specialist and probably more expensive forms of
accommodation with care. Quality of life needs to be thrown into the equation
by improving mainstream housing circumstances for all older people and
especially those on lower income and by investing in a wider range of housing
options including residential care.
Many
Canadian seniors are indeed aging in place.
Most are doing so out of choice.
However, in some instances seniors are staying put for other reasons
including a lack of affordable alternative housing options in their community. Statistics Canada recently reported that
housing affordability problems have actually increased for lower income seniors
between 1981 and 2001. This is contrary to the notion that seniors
are getting wealthier with each cohort.
The high proportions of seniors staying in their homes and their
neighbourhoods opens possibilities for creative ways to make sure affordable
supports are there when needed.
Linking
aging in place to the concept of home versus neighbourhood, the Australian
Housing and Urban Research Institute (www.ahuri.edu)
posted some interesting findings from a recent study
that examined the current housing tenure and future housing intentions of older
Australians. Drawing on a national
survey of nearly 7,000 older Australians, in-depth qualitative research using
focus groups and internet chat lines, the study found there is a significant
shift in the values and priorities of older Australians that is transforming
the patterns of future housing tenure, lifestyle and family relationships. One of the main points made by the study is
that independence, flexibility, consumer and lifestyle choices are now key
values and priorities for Older Australians. The study also found that aging in
place depends more upon attachment to location rather than the family
home. Older people are now accepting of
change with the baby boomers particularly comfortable with moving house. Problems of household and garden
maintenance, divorce, death of a spouse, downsizing, and lifestyle preferences
precipitate decisions to move.
Along
the same line, a recent report from the Joint Center for Housing of Harvard
University questioned whether tomorrow’s seniors, the aging baby boomers, will
have different needs, preferences and priorities in terms of their housing than
seniors of today. While today’s American seniors
overwhelmingly choose to remain in their own homes and neighbourhoods,
according to research cited in the report, aging baby boomers are expected to
be more mobile given their higher levels of education, greater wealth, better
health and broader travel experiences. However, just as is the case in Canada,
there is a widening gap between the most and least wealthy seniors in the US
spurring the need for more affordable housing options. The report also predicts a revolution in the
delivery of elderly support services (such as increases private sector in-home
help services and new assistive devises and equipment) to satisfy a generation
used to making their mark on the US economy and society.
A
nation-wide US study
found only about half of American communities had begun to plan to address the
needs of the exploding population of aging baby boomers. In response to this statistic, the National
Association of Area Agencies on Aging
produced a work plan to help communities develop an elder friendly
environment. A number of broad
solutions to the aging in place challenges were outlined including: how to
promote new housing options; transportation issues such as accommodating
suburban lifestyles and what to do when driving is no longer an option;
providing appropriate recreational opportunities; social, cultural and
educational enhancement; viewing seniors as economic generators; providing
access to health and social services; public safety issues and services; and
promoting universal design in the context of fostering a universal community.
According
to the National Association of Area Agencies on Aging,
the ten key components of an elder-friendly community are:
1.
Preventative
health care, such as health and lifestyle education, immunizations and
screenings, to reduce injuries and the onset of chronic diseases, as well as a
range of in-home health assistance to help people stay in their homes longer.
2.
Nutrition
education to promote healthy eating throughout a person’s lifespan, as well as
nutritious community-sponsored programs such as home-delivered meals for those
who have difficulty or are unable to prepare their own meals.
3.
Age-appropriate
fitness programs and recreational facilities that offer walking trails,
benches, fitness equipment etc…
4.
Larger,
easier-to-read road signage, grooved lane dividers, reflective road markings
and dedicated left hand turn lanes. Driver assessment and training to promote
safe driving for all ages, especially after strokes or other health incidences.
Transportation options for people who cannot or do not want to drive.
5.
Special
planning and training to help public safety personnel and other first
responders locate and assist older adults during emergencies and disasters.
6.
Home
modification programs that make necessary adjustments for people with special
needs. Zoning and subdivision plans that promote a variety of affordable,
accessible housing located near medical, commercial and other desired services,
as well as shared housing options for older adults and their caregivers.
7.
Tax
assistance and property-tax relief for those in financial need and programs to
protect older adults against fraud and abuse.
8.
Job
training, re-training and lifelong learning opportunities, as well as flexible
employment options to attract and retain older workers.
9.
Opportunities
to engage older adults in community boards and commissions as well as
purposeful volunteer activities in local government and non-profit
organizations.
10.
Single
point of entry for information and access to ALL aging information and services
in the community, and strategic expansion of necessary services to support the
older adults to age with dignity and independence in their home and community.
Along a
similar line, another recent report provided an international perspective on
policies for aging in place. Based on research conducted in Japan,
Finland and Australia, the report argues that well-designed housing and
transportation that links seniors to amenities and services are the most
critical components for positive aging in place.
Australian
researchers recently
added the viewpoint of seniors into the aging in place discussion. In addition to outlining the elements
(similar to above) of what would make a community senior friendly, researchers
had seniors rate which elements were most important for them. Rated top
priority was “personal/home safety”.
Other important elements for seniors were transportation, attitudes
towards seniors, physical attitudes and home support.
Seniors
in Ottawa were asked to rate this city’s quality of life in the 2004 Successful
Aging Ottawa’s Senior Survey. Issues of
most concern according to the rating scale were the lack of affordable housing
options for seniors, streets and sidewalks not being adequately cleared of snow
in the winter, concern that there are not enough home support services to allow
seniors to stay in their own home, and the level of responsiveness by local
government to the needs of older people in Ottawa.
Advocacy groups for seniors have tried to make the case for supportive
housing by linking housing to healthy aging.
For example, the Seniors Health Promotion Network in Atlantic Canada
recently made the following sweeping statement, “housing is the major variable
in an older person’s life, physically, socially, financially, and psychologically.” The report goes on to discuss the importance
of a supportive environment for “Aging in place” and promotes more government
involvement in stimulating affordable housing options for seniors. This theme is also echoed by an Ontario
report on supportive housing by the Toronto District Health Council.
A recent study
on the relationship between housing and the health of older seniors is worth
noting. Drawing on data from an
international survey of 1,918 people aged 75-89 years living alone in their own
homes in Swedish, German, British, Hungarian and Latvian urban areas, the study
found that participants living in better accessible homes, who perceive their
home as meaningful and useful, and who think that external influences are not
responsible for their housing situation (in other words they made their own
decision on where to live) are more independent in daily activities and have a
better sense of well-being. According
to the authors, the findings suggest that older adults should play the central
role in the negotiations around home modifications and relocation. Further, it is important that housing
solutions be included within a multidisciplinary approach to assessment and
care planning.
Another way to link housing for seniors and health is to examine the
relative risk to health of different settings. The results of a research trial
in New Zealand to improve
the outcomes of older people with high and complex needs found that the risk of
mortality to seniors living in the community could be reduced through a
coordinated service model. Three
different pilot “Aging in place” programs were studied: the first was a needs
assessment and service coordination initiative aiming to avoid duplication in
service provision; the second was a case management program which guides a
person’s pathway through the rehabilitation process; and the third was a
Flexible Integrated Restorative Team that aimed to provide restorative home
support for older people with high and complex needs. Some of the key findings of the research trial were:
- Older
people with high and complex needs who would otherwise be admitted to
residential care can remain living at home with no apparent risk.
- All
three pilot programs reduced the risk of mortality compared with usual
services.
- Caregiver
stress did not appear to increase in the intervention groups in comparison
to usual care.
- Predictive
modeling showed a number of situations where older people were more likely
to be hospitalized or enter residential care. These included functional
decline, social isolation, negative moods, caregiver stress, inadequate
meals, dehydration, delirium and a lack of medication review.
The bottom line conclusion was that older people assessed with high or
complex needs can safely remain at home with provision of appropriate
services.
In Canada, a number of studies have concluded that supportive housing
not only improves the quality of life of at-risk older people but has the
potential to prevent unnecessary institutionalization and decrease emergency
room visits. Using a pre and
post-program research design including a comparison sample, The Ottawa Aging in
Place Pilot Project
found that the introduction of a part time on-site tenant support coordinator
who linked residents to needed services along with a building dedicated home
making team made a positive significant impact on the lives of seniors living
in social housing. The study
reconfirmed the results of earlier research in Ottawa, which also employed a
rigorous longitudinal pre- and post-program research design. This model, however, evaluated the impact of
a public health nurse as the primary health care provider on-site full-time
five days per week, and examined impact on hospital admissions. Tenants residing in the buildings where the
public health nurse was present showed significantly fewer hospital admissions
than the controls in each year of the three years examined.
A similar recent similar study
conducted by researchers at Ryerson and the University of Toronto in
partnership with The Toronto Community Housing Corporation, Neighbourhood
Link/Senior Link, Etobicoke Services for Seniors and St. Paul’s LAmeroux added
further evidence to the field. The
researchers concluded that judging by the relative risks of seniors in the
study, supportive housing is a cost-effective alternative to
institutionalization, preferable in terms of quality of life and independence
even for the oldest old. In particular,
the authors of the study stressed the critical role of intensive case managers
in supportive housing in integrating services around the needs of the client,
substituting lower cost services (such as vacuuming, laundry, cleaning and
grocery shopping) for more expensive institutional supports, and reducing
demand on emergency services through ongoing assessments. The study also found that contrary to common
belief that given access to services people will maximize use and costs, under
intensive client focused case management the incentive was the reverse – to use
minimum level of services necessary to maintain the individual at the highest
possible functional status.
In the same vein, the evaluation of a recent demonstration program in
the US examined tenant outcomes for residents living in affordable,
service-enriched rental housing for homeless and those at-risk of becoming
homeless. After
monitoring the program for five years, the study found improvements in tenant’s
level of functioning, independence, general health, level of satisfaction, and
level of income.
Supportive housing in its more intensive form of assisted living has
been put forth as an alternative to more traditional institutional care for
seniors with dementia. The literature
search uncovered one academic paper that addressed this issue in relation to
quality of life. The study, based in Alberta, compared the effect of
specialized services on the quality of life of residents with middle- to
late-stage dementia living in assisted living facilities to those living in
traditional institutional facilities. The study used a prospective matched group
design that involved 24 long-term care centers and four assisted living
residences and 185 residents. The
researchers found that the assisted living group of residents demonstrated less
decline in activities of daily living, more sustained interest in the
environment, and less negative affect than residents in the traditional
institutional institutions. There were
no differences between groups of residents in the two settings in
concentration, memory, orientation, depression, or social withdrawal. The authors conclude that the quality of
life for adults with middle to late-stage dementia is the same or better in a
purpose built assisted living residence than in traditional settings.
A number
of recent reports on supportive housing have cited studies (Canadian and
International) that promote the cost-effectiveness of different models or
elements of supportive housing. In
addition, experts have tried to make the case that supportive housing and in
particular assisted living can prevent or delay admittance to higher cost long
term care and reduce hospitalization of seniors. It
has also been argued that targeted, managed home and
community care within an integrated continuum consistently meet individual
& system goals by maintaining the health, well-being and autonomy of
individuals and their caregivers and by helping to solve key health system
problems.
A frequently referenced program is On
Lok/PACE (Program of All Inclusive Care for the Elderly).
Initiated in the early 1970’s in San Fransisco’s Chinese community the program
has since expanded to 36 PACE projects in the US (Canadian equivalent in
Edmonton is called CHOICE). The service model, which targets seniors on low income
& high risk, is organized around adult day care services & offers a
continuum of services. Seniors are transported to the centre. Government
funding for PACE clients average 95% of the costs of institutional care.
Evaluations have shown that seniors enrolled in the program average fewer days
in hospital than comparable groups of seniors and experience better health
status & quality of health.
In terms
of Canadian research, evidence-based studies are fairly short in supply. Leading the field is Vancouver Coastal
Health (VCH). VCH continues to
examine ways to more cost effectively deliver health services. Through a series
of initiatives that included targeting the highest needs groups (complex care
seniors, adults with disabilities), linking community care funding to system
outcomes (e.g. ALC bed reductions) and shifting the focus from LTC beds to
assisted living (supportive housing) and residential care (care), VCH has
reduced residential care beds (25%-30% of community clients met residential
care thresholds), reduced ALC days from 12% to 6% and saved 17 in-patient beds
by introducing geri-triage nurses in all emergency departments (nurses who were
knowledgeable about available community support options).
A few other Canadian studies are worth noting. Hollander cited his own earlier study (2001)
of the cost-effectiveness of long-term home care that found over time, and for
all levels of care needs, home care, on average, was significantly less costly
than care in a long term care facility. Hollander also provided evidence on the
relative costs of home support and professional home care (e.g., nurses,
physiotherapist) in long term care. He
found that approximately 90% of the expenditures for long term home care, for
people with higher level care needs, were for home support services while 10%
were for professional services. This
means that any substitution effect of home care compared to facility care is,
in large part, due to home support services and indicates that even basic home
support services such as housekeeping can have a significant impact on the
cost-effectiveness of a health care system.
A recent report on the care of the elderly in Sweden
provided cost figures on the care of the elderly in regular housing and in
special housing. Sweden provides an array of publicly funded coordinated
services to seniors living in their own homes to assist aging in place
including meals, home adaptations, transportation, personal safety alarms, home
help, home medical services, short term housing, and day activities. Special housing exists for seniors who need
help arranging care and need 24 hour support. In special housing seniors
typically rent their suite which has been adapted for aging in place. On-site staff provides access to needed home
medical services. More and more seniors
in Sweden are able to live in regular housing with community support due to
advances in health and medical care.
The cost per care recipient in regular housing is approximately half
that in special housing. As well the
cost of providing special housing has increased more dramatically over the last
5 years than providing care in regular housing.
Hollander claims that there is now an emerging body of evidence on the
cost effectiveness of assisted living/supportive housing. He refers to several studies (Swedish,
British and American) that compare the costs, or costs and outcomes of assisted
living/supportive housing services with long-term care facilities. Hollander cautions, however, that the
evidence is still limited and somewhat mixed.
Most of the studies discussed in the Hollander report were based on very
small sample sizes, however, they do point in favour of supportive
housing/assisted living in terms of cost-effectiveness particularly when
adjustments are made for quality of life and client characteristics.
The SDR literature review also uncovered some research on cost
comparisons between different settings. A recent Quebec study compared the cost
and resources associated with disabilities of elderly people living at home, in
intermediate care (supportive housing) and in nursing care. The study found that the cost of care was
least at home and most in the nursing home setting, with intermediate care in
between. While this suggests that it
may be more cost effective to care for the elderly with disabilities at home or
in intermediate settings such as supportive housing, the authors caution that
the care was provided by less skilled people in the two less costly settings
and thus the quality of care must also be taken into account. The study did not measure quality of care.
Lessons
learned from evaluations of supportive housing for persons at-risk for
homelessness are also applicable for seniors supportive housing. A recent
outcome evaluation in Vancouver
examined changes in hospital utilization by individuals one-year post access to
supported and non-supported housing.
The study found that individuals with a mental illness who move into
supportive housing experience a significant decrease in hospital use in the
year post-housing. This decrease is
assumed to be linked to fewer admissions for psychiatric reasons as has been
shown by other studies.
The
evaluation of a recent demonstration program in the US examined tenant outcomes
for residents living in affordable, service-enriched rental housing for
homeless and those at-risk of becoming homeless.
After monitoring the program for five years, the study found improvements in
tenant’s level of functioning, independence, general health, level of
satisfaction, and level of income.
A recent
Canadian study by Pomeroy produced a costing analysis of different levels of
supportive housing for persons at risk for homelessness.
Pomeroy’s study tests the hypothesis that “purposeful, well designed supportive
housing is more cost effective than the cost of doing nothing which results in
either institutional or emergency use”.
Pomeroy collected data of actual costs across a range of existing
facilities and housing options in four cities – Vancouver, Toronto, Montreal
and Halifax. Pomeroy studied four levels of support and four building
forms. The study found that overall
costs were significantly higher for institutional responses versus community
residentially based options (even when a fairly high level of support was
provided in the latter). Emergency
services also tend to involve higher costs than the community/residentially
based options.
The
following ideas and best practices represent the most current thinking and
approaches related to supportive housing for seniors.
CMHC’s
report on the regulation of supportive housing for seniors provides some
interesting options. Responding to the study’s main finding that “all seniors
participating in the consultations felt that special regulation was necessary”
but not wanting to discourage developers from entering the field, the authors
of the report provided a range of options that could be considered by housing
policy makers.
- Option 1 – Develop a comprehensive supportive housing statute that would
include provisions related to:
- Rights
and responsibilities of residents
- Issues
relating to rental, purchase, and life lease tenure
- Mandatory
standards
- Special
standards in “assisted living”
- Information
to be provided to residents
·
Option 2 – Establish a system of “elder
ombudsmen” at
the provincial level with responsibility for seniors housing issues and would
serve as a “one stop shop” easy to access system for finding information,
making complaints and resolving disputes and other kinds of problems.
·
Option 3 – Establish a working group to
create national best practice guidelines such as the guidelines in the US for
assisted living facilities.
·
Option 4 – Establish a supportive housing
for seniors “centre of excellence” whose role would be to create a model “Code of Practice” for
accreditation.
·
Option 5 – Establish a (non-legislated)
system for accreditation with input from consumer and providers as well as academics.
·
Option 6 – Establish a central information database accessible through the internet
and through a seniors housing “hotline” that would provide information on
availability, costs, rules and conditions of residency.
SHIP is an excellent one-stop information port for seniors housing in
BC. The site includes information on
all types of purpose built seniors housing and has a separate section on
supportive housing and assisted living projects. SHIP has a searchable database available online at www.seniorshousing.bc.ca. SHIP could be a model for local
municipalities, other provinces or as national database as described in Option
6 above. SDR conducted the pilot
project for the establishment of a national database on supportive housing. At
this point in time the pilot database contains information on over 300
projects.
This
guide is an extremely useful tool for interested individuals and groups who
wish to develop and operate affordable, supportive housing for seniors. It is intended to assist groups ranging from
non-profit organizations that have never been involved in seniors housing
before to operators of large assisted living facilities. The guide focuses on housing that provides
hospitality services (meals, laundry, housekeeping, social and recreational
activities) or personal care services (help with bathing, dressing, eating
etc…) or both.
According
to the authors, supportive housing is considered “affordable” if it does not
require more than 70% of household income.
For seniors living on a minimum pension income, 70% equates to about
$700 per month. The authors maintain
that it is virtually impossible to provide shelter and services for $700 per
month without government subsidies.
Through research into existing supportive housing projects and
information gathered from a variety of other sources, the authors identify a
number of opportunities for streamlining costs and improving efficiency. The guide provides guidelines, comparisons,
and suggestions that will save money in the development, construction and
operation of supportive housing projects for seniors.
Topics
covered in the guide include: how to determine the need and demand for
supportive housing in your community; the development process, partnerships and
financing; board governance; operations: cost savings and creating
efficiencies; cost effective design; adaptive reuse; and developing supportive
housing for seniors in small communities and rural areas.
This
useful resource was recently produced by the Atlanta Regional Commission
jointly with the Community Housing Resource Centre of Atlanta. Aging in Place
is a tool designed to help local governments in the US (but could easily be
transferred to other countries) plan and prepare for their aging
populations. The tool recommends
techniques for coordinating housing development regulations and healthcare
supports so older adults can stay in their homes. It also addresses specific
quality growth practices so older adults can get out of their homes. It details examples of coordinated
approaches to the provision of neighbourhood housing and supportive services
that make it not only possible, but also cost effective for seniors to stay in
their communities.
The
heart of the Aging in Place toolkit is a set of local strategies organized into
three critical issue areas: Healthcare (Integration of healthcare delivery with
housing and planning initiatives); Environment (housing and urban design);
Planning and zoning (housing stock and location).
AARP
provides a check list for Aging in Place Home Modifications on their website.
Designed for use by elderly consumers, the site includes information on
understanding universal home design, a bathroom checklist, guidelines for
doors, floors and walkways, how to modify a kitchen, and information related to
lighting and storage areas. The site
also includes a special needs checklist which allows consumers to rate their
own needs for home modifications based on a range of difficulties with daily
activities. AARP studies have shown that medical costs of seniors living in a
Universal Design home can be as little as half the cost of living in a
traditionally designed home. For more information, visit www.aarp.org/families/home_design
Falling
is a risk factor for seniors in terms of losing their independence and having
to move to a nursing home. This report takes a comprehensive look at the issue
of falls among seniors. The report
includes a chapter on evidence-based best practices for the prevention of falls
including appropriate practices according to setting. Practices include: how to assess risk factors; using
multifactorial interventions that includes a combination of assessment and
interventions such as exercise programs, behaviour change, medication review
and modification, treatment of contributing health conditions, assistive and
protective devices, environmental modifications, and education. For more information about this publication
visit: www.phac-aspc.gc.ca/senior-aines/pubs/senior_falls/index.htm
Hollander,
in his 2006 review summarizes best practices for supportive housing within the
Ontario context. The practices are organized under four major components and
could be considered prerequisites for supportive housing:
- Best practices related to
philosophy and policy
- Fostering
independent living
- Client-centred
approach
- Assessment
and coordination of care and service
- Community
development
- Client
access to 24-hour support
- Emergency
response
- Security
checks
- Integration
within health care system
- Responsiveness
to health care system needs (e.g., in discharge capacity with hospitals)
- Best practices related to
service delivery
- Flexibility
in delivery in a variety of housing models
- ‘case
management’ functions of case finding, care/service coordination,
referrals and community development
- Providing
programs for all residents (e.g. congregate dining) to promote awareness
and create community
- Address
multiple client needs (e.g. frail, Alzheimer’s, mental health, cultural)
- Flexible,
consistent staffing
- Sensitivity
to multicultural and other client diversities and needs in recruiting,
hiring, training programs and education
- Accessible
communication tool for frontline staff (e.g., pager, cell phone)
- Best practices related to
administration
- Leadership
through common vision, commitment, and an understanding of seniors’ needs
and informed decisions
- Providing
specialized environments for special needs (e.g., Alzheimer’s)
- Funding
for all residents under one envelope or buildings in close proximity to
maximize flexibility
- Creating
efficiencies through critical mass
- Use
of client information management software
- Using
an internal waitlist for seniors in need of services
- Best practices related to
linkages and relationships
- With
all residents
- With
all housing providers for assessment, admission, ongoing reviews, and
other issues
- Access
and linkages to a larger range of services, including health and
long-term care
- With
hospitals and other formal health care service providers (e.g.,
physicians, clinics, outreach), other community service groups,
volunteers, local business, cultural organizations and networks
- Developing
alliances with other health care agencies providing related services in
the same building
This study focused on the development of a model for a
renovation and repair referral and advisory service for seniors and others who
are homeowners. The proposed model is intended to provide consumers with a
method for finding honest and qualified renovation and repair contractors. By
facilitating renovations, repairs and home adaptations, such an advisory
service could provide seniors with a better opportunity to age-in-place (i.e.,
to continue to live independently in their homes for as long as possible).
Converting single-family detached houses, owned and
occupied by seniors, to create secondary suites can have potential benefits for
seniors and the neighbourhoods in which they live. The objectives of this study
were to: estimate the interest of senior homeowners in converting their current
homes to create secondary suites; outline the financial and renovation
implications of conversion; and identify the regulations and zoning which
affect conversion. Findings are based on interviews with senior households and
group discussions with builders, real estate specialists and City officials.
(Prepared by The Council on Aging of Ottawa, Available from CMHC’s
Canadian Housing Information Centre, Order Number 65308)
These two publications are available in the Canadian
Housing Information Centre (613-748-2003).
They are an excellent resource for individuals and groups wishing to
learn more about the concept of flex housing and practical advice and how to
introduce flex design into home settings.
Flex design is an example of the type of building technology available
today that would assist aging in place.
This older (1998) publication is available in the Canadian
Housing Information Centre (613-748-2003).
It is still timely and provides a wealth of practical hands-on advice
including examples of needs assessment tools to help communities plan for their
aging population.
CMHC is
soon to release a number of reports that should prove useful for individuals
and groups planning to introduce supportive housing and aging in place
solutions. These include:
·
Supportive
Housing for Homeless and Hard-to-House Seniors, will provide an in depth
description of a successful housing project for homeless and hard-to-house
seniors with a focus on outcomes, lessons learned and advice for other
supportive housing projects.
·
Determining the Implications of the Aging of
the Canadian Population for Housing and Communities, will identify challenges and opportunities
for planning, designing and managing communities (cities, small towns and
suburbs) with increasing older populations.
The research will gather practical information through case studies of
communities that have already reached the proportion of seniors that Canada is
expected to have in the next 30 years.
·
Adapting Bungalows for Seniors’ Home Care, describes the results of a
post-occupancy evaluation of suburban bungalows that were redesigned for
seniors receiving health care services at home.
·
Adapting the Home Environment for
Alzheimer’s and Related Dementia, will develop a self-assessment tool that will function as a community
resource guide to individuals experiencing Alzheimer’s Disease and related
Dementia and their families through the process of adapting the home
environment while reflecting their individual needs and concerns.
·
Caring for Aging Parents, will provide research findings
to help the housing industry learn the degree of commitment that exists for
this type of personal family care for older parents and assess the implications
for the housing market of this form of housing demand.
·
Conversion of an Existing Institutional
Building to 58 Affordable/Accessible Housing Apartments for Seniors and
Disabled Adults,
chronicles the Armitage Gardens Project which revitalized a vacant and under
utilized portion of a building into 58 affordable rental apartments.
More
information about these reports and how to obtain a copy can be found in CMHC’s
Current Housing Research, Volume 13, Number 2, Winter 2006-2007 and by
contacting the Canadian Housing Information Centre at 613-748-2003.
The
following supportive housing initiatives have been referred to in the
literature and by experts. Some are
fairly new and some have stood the test of time.
WOODGREEN COMMUNITY CARE and WELLNESS FOR SENIORS
(Toronto)
WoodGreen
Community Services is a comprehensive neighbourhood service centre for
vulnerable people including seniors, families, youth, new immigrants, and
persons with special needs including the homeless. For seniors who need home support, WoodGreen offers: meals on
wheels; friendly visiting; telephone assurance/security checks; transportation
to and from medical appointments as well as group outings; personal support and
housekeeping services 24 hours a day, 7 days a week within seniors homes that
includes assistance with bathing, grooming, and taking medications; and
supportive housing that provides a social environment and 24-hour on site
support to assist seniors with their daily activities.
WoodGreen
also offers social activities and wellness programs, adult day programs for
seniors with dementia, case management and social work for seniors and their
families, and caregiver support.
Recently,
federal, provincial and municipal officials joined WoodGreen and its partners
for a ground breaking ceremony to celebrate the construction of a first of its
kind apartment complex (Wellesley Central Residences Inc.) that will provide
supportive housing to seniors and people with HIV/AIDS.
For more
information about Wood Green visit: www.woodgreen.org
Address:
835
Queen Street East
Toronto
Ontario
Contact:
Brian Smith, President, 416-572-0000, ext. 4001
LOFT (LEAP OF FAITH TOGETHER) JOHN GIBSON HOUSE SUPPORTIVE
HOUSING PROGRAM (Toronto)
The
John Gibson House Supportive Housing Program (J.G.H.) in the west end of
Toronto helps some of the most vulnerable, at-risk and frail older adults in
the community. Through a multi-service approach, the program offers 24-hour
on-site access to services for seniors who have traditionally been
under-served. JGH assists them with health and medical concerns, mental
illness, and substance abuse problems and other related issues. The communal
dining program at JGH provides affordable and nutritious meals to its
residents, and to seniors in the broader community. The use of Personal Support
Workers has provided practical assistance and care to residents, enabling them
to remain in their homes.
John Gibson House
provides supportive housing services for fifty seniors at its Crawford Street
site, as well as for seniors living at LOFT's apartment buildings in downtown
Toronto.
The success of the
John Gibson House Program is based on collaboration between its service users,
staff members, and the community. It has, for over 75 years, continued to be
committed to serving the needs of those most in need in the community.
For more information
about LOFT visit: www.loftcs.org
Contact: Maria Egervari 416-537-0001 or
(416) 537-3477; megervari.dunnav@loftcs.org
PEEL SENIOR LINK
Peel Senior Link, a non-profit charitable
organization established in 1991, provides a comprehensive range of personal
care & home-making services to seniors.
Its mission is to make independent living possible for senior citizens
who might otherwise be expected to enter more institutional settings, such as
Long-Term Care facilities and hospitals.
Peel Senior Link services have a reputation of being
client-directed, flexible and individualized. The organization coordinates
personal care & home-making services, at no charge, for over 1,000 seniors
in designated buildings in Mississauga and Brampton. These services include:
·
24/7
On-Site Services are for seniors who require daily and
ongoing assistance and live at one of the designated service buildings managed
by Peel Living and Wawel Villa. Having staff on-site lets seniors know that
help is available, easing their fears about living alone.
·
Personal
care & home-making services make it possible to
provide support to seniors without taking away their independence and dignity.
·
Day Services are for seniors who
require limited assistance on an as-needed basis and are available at all Peel
Senior Link designated service buildings.
·
Peel Senior Link strives to help
improve the physical health of seniors by providing education about nutrition,
helping seniors shop for healthier groceries, making referrals, and advocating
with community agencies on behalf of clients.
For more information about Peel Senior Link visit: www.peelseniorlink.com
Contact: Ray Applebaum, Executive Director: 905-712-4413;
ray@peelseniorlink.com
NORTH RENFREW LONG-TERM CARE CENTRE (Deep River)
The North Renfrew Long-Term Care Centre is a well known
rural project that includes 21 long-term care suites and 10 self-contained
apartments. Seniors are supported in
their apartments by a range of community support services including an Adult
Day Service – Drop-in Centre, Meals-on-Wheels-Wheels-to-Meals/Diner's Club,
Respite services, and transportation services.
The project is linked to other Deep River area health services including
the Community Care Access Centre, North Renfrew Family Services, Canadian Red
Cross Society Homemaker Services, and the Para-Med Health Services.
Address:
47 Ridge Road
P.O. Box 1988
Deep River, Ont.
K0J 1P0
Phone: 613-584-1900
LAURIER HOUSE and THE CAPITAL CARE GROUP (Edmonton)
The CAPITAL CARE Group has been caring for people since 1964.
The Group has the reputation of being
leaders in continuing care has grown into the largest publicly
funded and operated continuing care organization in Canada. The CAPITAL
CARE Group is a wholly owned subsidiary of Capital Health,
the regional health authority.
The Laurier House model is an innovative approach that
delivers, in a condominium-like setting, the level and type of health care and
social services that are traditionally available only in long-term care
institutions. Laurier House through
design and service arrangements allows individuals and couples to age in place.
One appealing feature is that elderly couples can remain living together in the
same apartment even when one partner needs more complex care. This is possible because Laurier House is
built on a health care campus that also
includes a traditional long-term care centre, built in 1994, and a centre for
Alzheimer’s disease built in 2001.
One of the unique features of the Laurier House model is
that it utilizes life leases to “unbundle” the costs of various services that
are provided, allocating them either to the client or the health care system.
Housing costs, a private expense, are separated from the costs of both publicly
funded personal support services and the housing-related support services. The costs of healthcare at Laurier House are
funded by the health region and clients must go through the same screening
process as they would to be admitted to a long-term care facility.
Laurier House is an attractive building with forty-two 1
and 2 bedroom suites. It is physically linked to the other two centres on the
campus. On the outside it has the appearance of a residential development and
inside it looks like a small hotel. At
the front entrance, a reception desk at the side lobby serves visitors to
Laurier House and the Alzheimer Care Centre. The Laurier House dining room
occupies a central location on the main floor and its kitchen operates like a
restaurant with limited hours.
The Laurier House model was recently (2005) the subject of
a CMHC study. This study examined the attitudes toward
life lease housing of Laurier House clients, their families, and the
professionals whom seniors consult when they require long-term care. The final report is available from the
Canadian Housing Information Centre, 613-748-2003)
CHOICE (Edmonton)
The Capital Care Group also operates three CHOICE programs
in Edmonton. In January 1996, Capital Health funded and introduced the
Comprehensive Home Option of Integrated Care for the Elderly (CHOICE). CHOICE was modeled after the American PACE
Program (Program of all Inclusive Care) which has been in existence since 1966
and was based on the On Lok Program in Chinatown in San Francisco.
The Edmonton CHOICE Program operated by a three way
partnership between Edmonton Capital Health, the Capital Care Group and The
Good Samaritan Society was the first of its kind in Canada. The program is designed to assist seniors to
continue living independently and in their own homes longer, by managing all
their health requirements. All
participants of the program come to one of the CAPITAL CARE CHOICE day centres
from one to five days where a full range of medical, psychological, social and
supportive services are available by a dedicated interdisciplinary care team.
More information about CAPITAL CARE COICE can be found at www.capitalcare.net/Programs/choice.htm
Address
The CAPITAL CARE Group
#500, 9925
- 109 Street
Edmonton,
Alberta, Canada
T5K 2J8
Contact:
Dr. Doris L. Milke, Research Coordinator
Phone
(780) 448-2400
Fax
(780) 496-7148
E-mail
info@capitalcare.net
Website Comments
info@capitalcare.net
Website
www.capitalcare.net
BEACON HILL VILLAGE (Boston)
Beacon Hill Village helps persons age 50
and older who live on Beacon Hill and in its adjacent neighborhoods enjoy
safer, healthier and more independent lives in their own homes–well connected
to a familiar and attentive community. Faced with the prospect of leaving the
neighborhood they love in order to obtain the services of a retirement
community, a group of long-time Beacon Hill residents decided to create a
better alternative–Beacon Hill Village is designed to make remaining at home a
safe, comfortable and cost-effective solution.
By partnering with proven providers of
services, Beacon Hill Village is able to offer its members preferred access to
social and cultural activities, exercise opportunities and household and home
maintenance services, as well as medical care and assisted living at home. As a
nonprofit, membership organization, it can provide these programs and services
more cost-effectively than most conventional retirement communities.
Villagers can choose from an à la
carte menu. Some services are included in the annual membership fee, with
others provided at reduced rates. Services include: Information services;
Household services (home repair, household cleaning, errands, organizing
closets, computer problem solving, bill paying etc.); transportation (individual and group
rides to anywhere – doctors, airport, friends, cultural events), meals and
groceries (weekly shopping, home delivered meals – elegant or casual, dining
groups), Volunteer programs (opportunities for members to help each and others
in the community at large), concierge services (delivered exclusively by one
in-home service provider and includes rides to anywhere, picking up
prescriptions, dry cleaning, packing boxes, mailing packages, waiting for
repair person, picking up theatre or concert tickets, taking in computer for
repairs, watering plants and picking up mail during vacations).
Beacon Hill Village originated
with a dozen civic-minded residents of this neighbourhood who all wanted to
remain at home even after experiencing some difficulties with activities of
daily living. Today the organization
has 340 members aged 52-98, an annual budget of $300,000, an executive director
and staff, a stable of established service providers and enough foundation
support to subsidize moderate or low income members who number one fifth of the
total. The annual fee for members is $550 for an individual and $780 for a
household, plus the additional cost of discounted à la carte services.
The grassroots experiment has
drawn praise in a recent AARP publication, has been written up in the New York
Times, and has been hailed by an array of research institutes, including the
AgeLab at M.I.T. and the North Carolina Centre for Creative Retirement. The organization has recently published a
how-to manual to help guide other community groups wishing to start a similar
organization through the complexity of creating a business plan and surveying
community needs.
Beacon
Hill Village
74 Joy Street
Boston, MA 02114
Phone: (617) 723-9713
www.beaconhillvillage.org
CERTIFIED AGING-IN-PLACE SPECIALIST (CAPS) PROGRAM
The
Remodelors™ Council of the National Association of Home Builders (NAHB) in
collaboration with the NAHB Research Center, NAHB Seniors Housing Council, and
AARP developed the Certified Aging-In-Place Specialist
(CAPS) program to address the growing number of consumers that
will soon require these modifications. While most CAPS professionals are
remodelers, an increasing number are general contractors, designers,
architects, and health care consultants
The CAPS program goes beyond design to
address the codes and standards, common remodeling expenditures and projects,
product ideas, and resources needed to provide comprehensive and practical
aging-in-place solutions. CAPS graduates pledge to uphold a code of ethics and
are required to maintain their designation by attending continuing education
programs and participating in community service.
A Certified
Aging-in-Place Specialist (CAPS) has been trained in:
- The unique needs of the
older adult population
- Aging-in-place home
modifications
- Common remodeling projects
- Solutions to common barriers
More information about CAPS can be obtained
from The Remodelors Council at 800-368-5242 x8216 or via e-mail at remodel@nahb.com
The 2004
Successful Aging Ottawa Survey and the 2004 Ottawa Fact Book on Aging along
with the BC guide by Mancer & Holmes (70 Ways to Reduce the Cost of
Developing and Operating Supportive Housing for Seniors)
provide the type of information that will help local housing and service
planners determine the need for supportive housing in Ottawa. Using just two
indicators from the SAO Seniors Survey – the number of respondents who could be
considered frail (based on perceived poor health, number of poor health days in
the last month, need help with 3+ ADLs or rely on Para Transpo) and the number
of respondents on low income (<20K and no greater than 30K), it is estimated
that somewhere between 1000 and 4000 Ottawa seniors could benefit from
affordable supportive housing. For
seniors with an annual income of $20,000 the most they could afford for housing
and support services would be $1,170 per month. (Based on the affordability
guidelines provided by Mancer & Holmes)
Previous
research has identified unmet needs for older homeless women
and gay, lesbian, bisexual and transgendered seniors in Ottawa.
Next to
Calgary, Ottawa has the fastest growing senior populations in Canada, a
population that is projected to increase even more rapidly over the next few
decades. The number of seniors 65+ in Ottawa (almost 90,000 now) is expected to
grow to 267,000 in the next 30 years and the group 85 and over will more than
triple and stand at nearly 34,000. Whereas today, seniors represent about 12%
of the population by the year 2031, about one quarter of the population will be
65+. The reason for this surge in
numbers is due largely to the aging of the “baby boom” generation born between
1946 and 1960. Increasing longevity and
declining fertility rates among the child-bearing population are also factors.
There is
much debate among experts
about the implications of an aging society in Canada. In particular, questions
such as: “Will baby boomers be better or worse off financially during their old
age than previous generations?”and “How well will baby boomers age in terms of
their health?” are often posed. The
answers to these questions will impact housing, health and social services over
the next 10 to 20 years.
Some of
the most recent projections and “thinking” from experts at Statistics Canada,
National Advisory Council on Aging (Seniors in Canada, 2006 Report Card),
National Council of Welfare, and universities across the country suggest the
following trends:
·
The
percentage of seniors living on low income has decreased over time and it would
appear that each cohort of seniors over the past 4 decades have had more
disposable income. At the same time, an increasing number of people in the
“boomer” generation are feeling uncertain about their financial future and do
not know when they will be able to retire. Over thirty percent of recently
surveyed baby boomers (General Social Survey, 2002) were not sure when they
would retire.
·
The
percentage of seniors who are currently working has increased from 6% in 2001
to 8% in 2006, a trend that is predicted to continue for a number of reasons
including declining high tech stock prices in pension plans, the mounting
pressure on the labour force due to the early retirement of some baby boomers,
coupled with a booming economy in many parts of Canada. In a recent Statistics
Canada Labour Force Survey (2002), one fifth of Canadians reported that they had no plans for retirement and
expected to continue working after age 65.
·
There
is a widening gap between families at the top of the income scale and those at
the bottom with respect to pension contributions. Those at the top of the scale
are better off than their 1986 counterparts than those at the bottom. This
trend held true for two parent families as well as lone parents and singles.
·
The
increasing longevity of Canadians is putting pressure on pension funds,
particularly the huge size of the Baby Boomer generation. Recent immigrants who
are less likely to have a pension plan through employment and are more likely
to be self-employed, as well as women living alone are most vulnerable to the
experience of financial insecurity in retirement.
·
Income
is related to physical and mental health and overall quality of life (a
relationship confirmed in the 2004 SAO Seniors Survey). While the average
income for seniors has improved over time, the income gap between men and women
continues. According to the National Advisory Council on Aging, senior women
living alone, older seniors 75+ and recent immigrants are more likely to live
on low income than other Canadian seniors (also confirmed in the 2004 SAO
Seniors Survey).
·
The
percentage of seniors who own their own home has increased over the last 5
years with 86% of couples owning their own home in 2003. With more and more senior homeowners, the
potential for needed home maintenance and other home support services
increases.
·
Seniors’
housing conditions in general are improving with fewer seniors living in core
housing need (paying more than 25% of their income on housing) now than six
years ago
·
The
number of seniors living alone is on the rise, particularly for women over the
age of 85.
·
As
the baby boomers age, the number of people in the “sandwich” generation
continues to rise – almost 3 in 10 Canadians aged 45-64 in 2004 reported that
they were caring for a senior and also had at least one unmarried child living
at home. Eighty percent of these
Canadians, mainly women, also work outside the home causing 10% of these
working Canadians to reduce hours and lose income. (According to the 2004 SAO
Seniors survey, as many as 3000 seniors in Ottawa may be caring for an ill
spouse as well as still supporting adult children.)
·
The
projected health of “baby boomer” seniors has been given a mixed grade. It is
true that life expectancy continues to rise. More and more Canadians are
embracing a healthy lifestyle (witnessed by an increase in the reported
operating revenue of fitness and recreation centres) resulting in improved
functional and mental health. As well, the introduction of cholesterol lowering
drugs and other medical breakthroughs have seen a decrease in heart
disease. At the same time, however,
other indicators are not so positive. Baby boomers have a higher rate of
obesity than previous generations (more for men than women). As a result, the
rates of chronic diseases such as diabetes and arthritis are on the rise.
·
Today’s
seniors are embracing technology with a growing percentage (5% in 1997 to 25%
in 2003) using the Internet. In the
2004 SAO Survey 40% of respondents
reported using the internet for Email and other purposes. This percentage will
continue to grow tremendously as baby boomers age. According to Statistics Canada, Ottawa has one of the highest
Internet usages in Canada with 77% of the population (85% age 18-44) reporting
use of the Internet in 2005.
Canadian
Centre for Elder Law Studies, A Legal Framework for Supportive Housing for
seniors: Options for Canadian Policy Makers. Prepared for Canada Mortgage and
Housing Corporation, March 2005.
Seniors
Health Promotion Network, More Than Shelter: Housing Policy Kit for Seniors in
Atlantic Canada, 2004.
Social
Data Research Ltd., Supportive Housing for Seniors. Prepared for Canada Housing
and Mortgage Corporation, 2000.























